PEER REVIEWED
A Novel Approach to Clinical Education
through Distance Learning
Stephanie L. Adams, OD, PhD, and Elizabeth Wyles, OD, FAAO
Abstract
The circumstances of coronavirus disease 2019 (COVID-19) drove the development of a novel teaching methodology for optometric clinical education using distance learning. In small groups students conduct a virtual clinical encounter in real time while educators observe. As they would in an actual patient encounter, students exercise clinical reasoning as they elicit case history, request and interpret tests, consider differential diagnoses and compose management plans. Additionally, students deliver patient education using video sharing. This methodology transforms clinical education using a closely monitored, interactive clinical learning experience with detailed feedback, which has benefits beyond those available in traditional clinic.
Key Words: distance learning, clinical education, teaching methodology, virtual clinical encounter, simulated patient, simulated clinic
Background
During the unprecedented circumstances of the coronavirus disease 2019 (COVID-19) pandemic, professional education was forced to shift to distance learning to maintain student safety and limit the spread of disease while still advancing the students through the curriculum. The interruption of clinical encounters was arguably the greatest challenge for the continuation of optometric clinical education. Novel uses and adaptations of technology surged in the health professions so that clinical training could continue remotely.1-6 The virtual clinical encounter (VCE) described here is one such novel adaptation. It creates an interactive learning experience using student collaboration, learner-generated content and detailed discussion.
The use of patient simulation in clinical education predates COVID-19. Simulated patient encounters in higher education, most commonly in schools of medicine and nursing, have been increasingly utilized to foster student collaboration, support learning outcomes and improve patient outcomes and survival.7-12 A wide variety of simulation methods are used to create realistic clinical scenarios, from computerized mannequins to virtual patient role play.7,8,12 Simulated patient encounters offer students engaging clinical experiences to build skills in a safe and supervised environment at reduced costs compared with standardized patients played by actors.7,10 Close monitoring of the simulated clinical experience by educators allows them to provide valuable feedback to help students connect theory to practice, a requirement for success in clinical practice.10
Although computer-based clinical activities have been described in optometric education, their complex methodology using custom-developed software is not readily reproducible, making adoption by other institutions difficult.11,13 To guide the needed expedited development of virtual clinical activities, a search for peer-reviewed methodologies in the Education Resources Information Center (ERIC) via an EBSCO database was conducted using terms “optometry simulated patient,” “optometry patient simulation,” “optometry patient simulator” and “optometry virtual patient.” The search revealed no relevant optometric teaching methodologies since 1990 when problem-based learning was incorporated into the optometric curriculum.14 The lack of an available optometric patient simulation method led to the realization of the need to develop a technology-based VCE in order to continue clinical education during required social distancing in Spring 2020.
When incorporating technology into education, the SAMR (Substitution, Augmentation, Modification, Redefinition) model can be used to predict overall impact. The SAMR model of technology integration describes enhancement of existing teaching practices using technology that leads to the conception of new methodologies not previously possible.15 While originally described for use in K-12 programs, this hierarchical model has been applied in higher education including optometry.16 The enhancement areas of substitution and augmentation introduce a technological element that does not significantly alter the original activity. Substitution simply replaces a learning activity with a technology-based tool without functional change, such as using digital instead of paper study guides. Augmentation describes implementing a technology-based tool that results in a functional advantage, such as the use of online recorded lectures available for review with adjustable playback speed. The transformative areas of modification and redefinition require a higher level of task design inducing student collaboration and resulting in new learning experiences. Modification describes substantial redesign of a learning activity, for example, using a 3D anatomy mobile application for students to each learn a bone of the orbit and then teach their peers. The highest level of the SAMR model, redefinition, creates new tasks not previously possible, such as developing an interactive virtual patient encounter. While some caution that overemphasis on technology may distract from teaching, the SAMR model framework leads to novel learning activities that are possible only with the use of technology.16,17
The demand for a fully remote clinical education combined with an understanding of previously accepted simulation and technology-based pedagogies in professional education fueled the development of the VCE for optometric student clinicians using videoconferencing, student collaboration and learner-generated content. The intent of the described methodology is for students to apply procedural and didactic knowledge in a closely monitored simulated patient encounter using critical thinking and clinical reasoning, and to enhance these skills using detailed feedback. Although the VCE was born out of necessity, incorporating this interactive activity into traditional clinical education provides an opportunity to develop students’ clinical reasoning skills leading to improved clinical competency.
Methods
The VCE is currently utilized for second- and third-year students enrolled in primary care optometric clinical training. Students in groups of four to six conduct a VCE within a predetermined time limit consistent with their level of training. The entire activity spans two remote clinical sessions and uses additional assignments to be completed outside of clinic time (Figure 1).

Figure 1. Outline and brief description of virtual clinical encounter (VCE) activities. Click to enlarge
The VCE is conducted in real time using videoconferencing, which concludes with students composing a formal assessment and management plan in a shared online document during the first clinic session. Following completion of the VCE, each student clinician records his or her patient education using video sharing. (Second-year student’s initial patient education on allergic conjunctivitis following a VCE in week 1.) Peers and preceptors review the patient education videos during a subsequent discussion session. After the discussion session, students re-record their patient education videos. (The same student’s second attempt at patient education on allergic conjunctivitis after the discussion session in week 2.)
Instructions to students
Students are required to enable their audio and video features in the videoconferencing application to ensure all are actively participating. Suggested time for the VCE may vary from 45 minutes to 2 hours depending on student clinical skill level and case complexity. Students receive the following instructions at the start of the activity:
For your virtual clinical encounter (VCE) you will be working together as a group. You have 1.5 hours to conduct an eye exam on your patient, so please keep track of time. Have paper and a pen or equivalent ready to record your exam findings as no digital or hard copy will be provided. You need to give the patient instructions, verbalize equipment setup, and verbalize your exam findings for each procedure. Your group should work together and discussion is encouraged as you move through the exam. The group must unanimously agree to obtain each test or procedure requested. For example, if one clinician mentions they want to obtain a macular OCT, it is not provided unless all group members verbally agree. All requested information will be presented in images or videos for your interpretation. In your VCE you do not consult with a preceptor. Only perform the tests you consider necessary, keeping efficiency in mind.
At the end of the exam, the group must reach a consensus to release the patient after all requested tests and questions have been answered. The group should then compose an assessment and management in Google Docs to be completed before you leave the session. Evenly divide the assessments you have determined across the group members. Each group member will be responsible for providing the corresponding patient education for their assigned assessment in a recorded video on Flipgrid, due within 48 hours of the session. Your Flipgrid videos will be reviewed by your group and preceptor during the discussion of your clinical performance next week.
Faculty and session responsibilities
The first clinic session ideally uses two educators to facilitate the VCE. One educator (educator #1) plays the voice of the patient and presents the prepared album of case images and videos as requested by the student clinicians, while the other educator (educator #2) takes detailed notes and serves as overall facilitator as needed. A comfortable environment is needed for the students to verbalize their thought process during the VCE. In less vocal groups educator #2 may need to intervene, interrupting the student autonomy of the activity, in order to facilitate discussion or next steps. Emphasizing detailed VCE instructions, including the requirement for students to verbally request needed tests, instruct the patient and state the exam findings, are important for stimulating continued student discussion. As the exam unfolds, students may need to be notified of limitations in available equipment in order to redirect them to the most meaningful tests. For instance, with no available autorefractor, students are guided to perform retinoscopy. The educators must remain cognizant of the VCE instructions, letting the students verbalize equipment setup and patient instructions before revealing the indicated image or video. Educator #2 documents a thorough transcription-like record of the VCE, including but not limited to individual student contributions to case history, patient communication, sequence of procedures, ancillary test selection, interpretation of presented data and application of knowledge as it relates to the formulation of diagnoses and associated management.
In the second clinic session, educator #2 facilitates the discussion forum to evaluate the VCE record of student performance and review the students’ patient education videos. During the discussion the students are encouraged to carefully consider their choices regarding efficiency, test selection, diagnosis and management. This encourages them to critically evaluate their clinical decisions and knowledge base in a constructive environment. This type of discussion allows for the optometric institution’s clinical evaluation rubric to be followed when assessing the students’ performance in the VCE.
Purposeful pairing of faculty, such as clinicians from different specialties or a junior clinician with an established faculty member, may encourage more comprehensive and creative case content as well as foster faculty development. Pairing a basic science educator with a clinical instructor may also be advantageous. If utilizing two educators is not feasible, a teaching assistant may be an excellent resource, replacing educator #1, to help facilitate the VCE. Alternatively, if using a single educator for both roles, the VCE can be recorded and reviewed later in preparation for discussion.
Distance learning platforms
The technology required to successfully facilitate a VCE includes a videoconferencing platform, a slideshow presentation tool, an online shared document with real-time editing capability and a video-sharing application. While many tools are available for performing these tasks, the authors use the following platforms.
- Zoom (Zoom Video Communications, San Jose, Calif.). Videoconferencing hosts the student group and facilitates the presentation of requested image and video-rich exam data as the students navigate the VCE. Videoconferencing is also needed for the detailed discussion and review of the patient education videos the following the clinic session. Zoom is an affordable online software platform for virtual communication in video, phone or chat form, which the authors use to facilitate the activities. In Zoom’s “gallery view” all participants can visualize and communicate with each other simultaneously using their electronic device’s camera and microphone. During the VCE, educator #1 uses the screen-share function to present the exam data according to the students’ requests. Importantly, the Zoom videoconference can continue without the host present, as both educators will eventually exit to allow the students to complete the associated VCE assignment as a group.
-
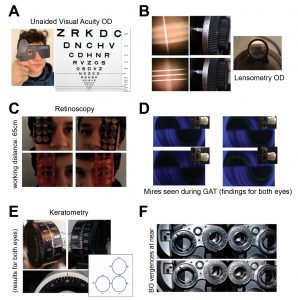
Figure 2. Examples of VCE album images presented for student interpretation and documentation. (A) The image for unaided visual acuity at distance is presented as educator #1 reads the appropriate letters with planted errors. (B) Once the student clinicians request lensometry of the habitual glasses, the group is presented with the sphere and cylinder mires, drum and axis wheel reading. (C) Retinoscopy findings are presented with the neutralizing lenses highlighted. (D) A variety of Goldmann tonometry mires seen during the applanation process are presented; students must select the correct alignment to record the accurate reading. (E) Keratometry readings are presented with the horizontal and vertical drum, axis and illustrated mires. (F) Base-out vergences at near, performed in the phoropter, are presented after students properly describe the equipment setup and instruct the patient; educator #1 reports “break” (F, top) and “recovery” (F, bottom). Click to enlarge
PowerPoint (Microsoft Corporation, Redmond, Wash.). A slideshow presentation organizes the VCE-associated album of image and video exam data. The authors use PowerPoint to organize all potential exam components the students may request as it allows for image animations and video embedding. Each slide houses a specific exam procedure and/or result. Educator #1 operates the PowerPoint album, which is organized in a logical sequence to aid in navigation and presents the necessary slides with Zoom’s screen-share function. The entire VCE is composed of images and videos of exam findings, presented only after students correctly instruct the patient and describe the equipment setup. The students view each requested test individually while the entire VCE album remains hidden. As educator #1 voices the patient’s response throughout a procedure, the corresponding image is presented (Figure 2). In many exam procedures the slide uses animations to present images sequentially according to patient responses, for instance, when reporting “blur” and “break” in vergence testing. Students are not given hard or digital copies of exam data. To mimic an actual clinical experience, the case images and videos are presented temporarily and the students are expected to record the interpreted data. Each group’s unique navigation through a VCE may result in unseen slides for the data that is not requested. A complete case and the associated VCE album are provided here for review and application to clinical education.
- Flipgrid (Microsoft Corporation, Redmond, Wash.). A video-hosting platform enables students to record their patient education at the conclusion of the VCE. Flipgrid is an online social engagement tool that uses video sharing to house educator-posed topics that collect learner-generated content in response. Flipgrid also allows peer feedback in video response. The authors use Flipgrid to host the students’ patient education videos. Flipgrid offers a customizable time limit for each video, which the educator controls. The authors use a 90-second time limit for the students to record their patient education, performed as if the patient is sitting in front of them. During the discussion session, the students’ patient education videos are viewed and evaluated for the key components of patient education, including but not limited to appropriate language, exhibited sensitivity, explanation of diagnosis, prognosis, use of educational materials, communication of management and treatment options and overall professionalism.
- Google Docs (Google LLC, Mountain View, Calif.). A shared online document allows students to compose their assessment and management at the conclusion of the VCE once the patient is dismissed. Google Docs is an online-based word processor that allows for real-time collaborative writing and editing. All users are able to see individual contributions and changes as they work towards a final document. The authors create Google Docs in advance, which are shared with the students in the videoconference chat during the first clinic session, taking precaution to prevent other student groups from viewing the document.
Case format
All exam findings are presented in images or videos, which can be easily acquired using cell phone cameras and readily available optometric equipment. Gracious colleagues or family members can pose as the patient in the necessary images and videos using basic equipment such as the occluder and the diagnostic kit. For fundus photos and more sophisticated ancillary testing, de-identified images from a clinical database may be utilized.
The VCE-associated case is composed by the educators, a collaborative effort with key points pulled from past clinical experience and in alignment with the didactic curriculum. Highlighting exam nuances that students find challenging due to low encounter frequency or higher level of required clinical reasoning may prove beneficial. Careful content development is required as the educators must predict the various avenues students may logically take to conduct the exam. An album of clinical images and videos specific to the case is compiled to accommodate requested testing within reason. Any illogical testing requested by the students may otherwise be deemed not relevant to the case, or students may be given a verbal account of the expected finding if needed. Realistic obstacles can be incorporated for the students to overcome, such as the need to use auxiliary cylinder lenses in the phoropter.

Figure 3.The VCE is conducted in Zoom using the screen-share function. A “gallery view” of five student participants is seen on the right as they trial frame the manifest refraction at near. The students ask about the patient’s visual comfort and check near acuity using the presented near card. Educator #1 uses the case script to respond and read the appropriate letters with planned errors, letting the students determine and record the correct acuity. Click to enlarge
The educators determine the case details and patient responses prior to the VCE (Figure 1). Creating a script outlining the chief complaint, ocular, medical and family history, visual acuity, refractive status and pertinent exam findings is essential for case consistency and ease of response for educator #1. For instance, to assess visual acuity educator #1 (the patient) is instructed by a student to “cover your left eye and read the lowest line of letters you can see.” Educator #1 responds by reading the presented eye chart at the predetermined acuity level, including purposeful errors, allowing the students to determine the correct final acuity (Figure 3).
In the VCE no preliminary data is given. The encounter begins with a patient photo and his or her age. The students are not provided with an exam template, ensuring that data is not indiscriminately collected and encouraging them to use exam results to determine additional necessary tests. The VCE requires the students to be knowledgeable about efficient clinical practices, including eliciting case history, properly instructing the patient, correctly interpreting test results and utilizing necessary ancillary testing. For example, a fundus image with a peripheral retinal hole should alert the student to request scleral depression and ask the patient about pertinent symptoms. To increase student clinician responsibility for the encounter, the students compose their formal assessment and management at the conclusion of the exam, including the final spectacle prescription, required follow-up and signing the virtual chart.
Discussion and review of the virtual clinical encounter
During the second clinic session, which is led by educator #2, the students re-experience the simulated exam in an open discourse with the educator, where level of efficiency, testing choices and pertinent concepts are addressed. The discussion is guided by the transcription-like record of the VCE, created by educator #2 during the prior session, along with the students’ submitted assessment and management. Strengths, opportunities for improvement, weaknesses and any missed diagnoses from the VCE are discussed. Students exercise critical thinking as they are asked to support or retract inefficiencies and missteps. This somewhat informal discussion also allows the students to ask questions to their peers and preceptor regarding clinical judgement and individual practice styles.
After the conclusion of the exam discussion, the students’ patient education videos are viewed by the group and educator using screen share in the videoconference application. Each student in turn states a positive characteristic and a potential area for improvement for each group member’s video. Any key points not mentioned are highlighted by the educator. The students are then assigned to re-record their patient education in Flipgrid, applying the feedback received. Their peers later post additional feedback for each re-recorded patient education via video response in Flipgrid (Figure 1). In future VCE cases re-recordings can be assigned as needed.
Discussion
Using technology-enhanced distance learning, the VCE allows student clinicians to conduct a simulated comprehensive eye exam. When considering its educational impact using the SAMR model of technology integration, the VCE falls within the transformative areas of modification and redefinition due to the creation of an interactive virtual patient encounter experience that provides benefits beyond those available during in-person clinical encounters.15 This methodology allows the educators to witness the unfolding of the student-led exam, mimicking an observed student clinical encounter yet avoiding the student anxiety of direct observation by a preceptor in front of an actual patient. The educator gains an unparalleled view into the students’ clinical judgement and an opportunity to enhance student clinical reasoning through detailed feedback and discussion. Unique advantages of this novel clinical education methodology include emphasis on clinical reasoning, purposeful content design, refinement of patient education skills, peer collaboration and comprehensive assessment in alignment with traditional clinical grading rubrics.
A common obstacle for professional students is the shift in mindset from simply collecting data to critically analyzing data to efficiently and successfully navigate an exam. Clinical reasoning is an acquired skill that can be learned in the context of a clinical encounter, real or simulated.18-21 The gap between students’ translation of theory into clinical competency is likely a result of passive learning without sufficient application of critical thinking, which is required for successful clinical reasoning.18-21 The VCE creates learner-guided case history and test selection, preventing the students from relying on a preset exam template. Using a problem-based approach, the students must choose appropriate ancillary tests based on the evolving clinical findings throughout the encounter. This encourages students to exercise clinical reasoning throughout the VCE as they consider the case history and exam data to make the correct diagnoses.
Traditional learning cases are passive exercises when considering data collection. Cases presented in the Patient Assessment and Management (PAM) format of the National Board of Examiners in Optometry (NBEO) Part II exam prevent students from practicing ongoing analysis during data collection, but instead present all data necessary to establish the diagnoses and finalize treatment and management. Clinical reasoning in these exercises is limited to data analysis for diagnosis and appropriate treatment and management at the end of a reviewed case. In contrast, the VCE is designed for students to actively reason through case history, test selection, modification of exam techniques and data interpretation throughout the simulated exam in order to arrive at the appropriate diagnoses. If the students collect insufficient data during the VCE, the diagnoses may be incorrect or missed. The educator observes the students’ clinical judgement during these processes to comprehensively assess their level of clinical competency and identify areas for improvement.
As opposed to the somewhat haphazard development of students’ strengths according to the sequence of clinic patients and/or specialties they are assigned to for their in-person training, a series of VCEs can be systematically designed at the appropriate level of knowledge base and corresponding clinical reasoning in parallel with the didactic curriculum. Utilizing incrementally advancing topics in VCE cases creates continuity of learning as the students draw from past discussions, allowing the educator to easily observe student growth over time. Subsequent VCEs show incorporation of prior discussions leading to increased efficiency, critical thinking and clinical reasoning. In the short course of VCE implementation thus far, weekly gradual improvement has been demonstrated by each student. Importantly, VCE cases may be further developed to expose students to low-frequency but high-criticality cases they may not encounter during their training. This includes conditions such as giant cell arteritis and acute angle closure, where proper management can be life and/or vision-saving. Exposing students to simulated patients with critical conditions improves their management skills, preventing errors when these emergent situations arise in clinical practice.7,8
Adding a skills component to the VCE, each student records their patient education using a video-sharing platform. Incorporating social media into structured education often creates learner-generated content, promoting student engagement and active learning, which can also be monitored by the educator.22-24 The social media video-sharing tool Flipgrid provides a secure outlet for students to practice and refine their patient communication and education skills, a key aspect of successful optometric practice. This activity is used to examine the students’ professionalism, level of sensitivity, appropriate use of language, description of management and treatment options and effectiveness of communication style, consistent with the evaluation metrics of the NBEO Part III Clinical Skills exam. Patient communication skills, typically only refined over time during actual patient encounters, are arguably the foundation of the doctor-patient relationship and a key factor in positive patient outcomes.25 The VCE creates a unique opportunity for students to develop these skills using a supervised simulated patient, rather than an actual patient.
The small group format of the VCE facilitates learner-guided collaboration. Students are able to share their strengths, learn from peers, engage in friendly debate and exhibit leadership as the group conducts the exam. Each student group’s particular navigation through a VCE results in variations in the elicited case history, selected tests and final management decisions. The students may or may not collect the necessary data to determine the correct diagnoses by the end of the exam. For example, once the simulated patient is dilated, the students can no longer assess the patient’s accommodative status when attempting to finalize the glasses prescription. While some errors are realized during the VCE, others are missed and need to be identified in the discussion session. The second clinic session is used to provide timely feedback in a structured discussion, which is important to the success of small group learning.26 The educator’s discussion is personalized to each student group, utilizing the transcription-like record created during the first clinic session to address individual strengths and opportunities for improvement.
Consistent with the VCE’s intent, students apply procedural and didactic knowledge while practicing critical thinking and clinical reasoning throughout a simulated patient encounter. Thus, the VCE allows the educators to apply a traditional clinical grading rubric in distance learning, including evaluation of clinical skill, analysis, judgement, communication and professionalism. In a VCE students have an equal opportunity for success in their clinical evaluation using a common simulated patient, whereas in actual clinic individual patients influence student evaluations according to variable exam complexity. Additionally, the educator’s transparent observation of student clinical competency more accurately reveals the student clinician’s level of proficiency as the simulated exam unfolds. As the educator hears the students’ thought processes, the causes of decreased efficiency such as unnecessary testing or gaps in knowledge are more easily identified. This thorough assessment of student clinician performance allows for detection of critical student errors that may go undetected in traditional clinic, such as poor endpoints in tonometry mire alignment, which are revealed and corrected in the subsequent discussion session (Figure 2).

Figure 4. A sample of unsolicited positive student feedback on the VCE, which was received via written comments in end-of-quarter faculty evaluations and in direct e-mails to the educators. Click to enlarge
The lack of motor skills assessment, not feasible away from clinical equipment, is the greatest limitation to the described clinical education methodology. However, this allows for emphasis on development of critical thinking skills leading to stronger clinical reasoning, which is the more challenging skill to teach.18-20 While the VCE requires careful content development, which may be time-consuming, the activity can be reused with new student groups and may be expanded into follow-up visits of the same simulated patient, building on the students’ previously submitted assessment and management. Although the VCE is only modestly technologically sophisticated, this allows for adoption into any existing optometric curriculum with educators who are willing to learn the platforms used. Future enhancements in this methodology may include the use of simulated telemedicine for more realistic patient interaction.
An overall positive student attitude towards the VCE was captured in unsolicited student comments received in the authors’ faculty evaluations and e-mail exchanges with students. The informal feedback showed student appreciation for the identified gaps in their knowledge, exercises in critical thinking, patient education skills practice and personalized group feedback (Figure 4). Although quantitative outcome measures are needed to validate this methodology, improved student performance was readily observed after only a few VCE and discussion sessions.
Conclusions
The VCE transforms the traditional clinical education experience into a controlled clinical learning environment using a novel distance learning methodology with simulated patients. The VCE provides opportunities to improve student clinical performance beyond those available using traditional case analysis and in-person precepted clinical encounters. Due to the educator created content and detailed feedback, this methodology helps to close the gap between theory and clinical competency. The VCE promotes improved clinician efficiency, knowledge base, critical thinking and enhances clinical reasoning. Additionally, the video-sharing component enhances patient education skills using learner-generated content and individualized feedback from educators and peers.
The VCE has been well-received by students with obvious overall improvement in clinical performance noticed by both educators and student clinicians. While born out of necessity to continue clinical education during social distancing, long-term the VCE may serve as a preparatory activity for clinic, adjunct to clinical education, elective clinical education course, patient education training activity, and/or facilitate clinical remediation.
Acknowledgements
We thank Lindsay Sicks, OD, FAAO, for providing de-identified tomography images and expert guidance in interpretation, which were key components of the virtual clinical encounter album.
We thank Navjeet Randhawa, Class of 2022, for sharing his patient education videos (https://vimeo.com/424974833 … and … https://vimeo.com/424975531), and Ethan J.K. Wyles for his participation in key photography for the virtual clinical encounter album.
Disclosure
The authors declare they have no financial interest in any of the companies mentioned in this paper to disclose.
References
- Codispoti CD, Bandi S, Moy JN, Mahdavinia M. Running a virtual allergy division and training program in the time of COVID-19 pandemic. J Allergy Clin Immunol. 2020 May;145(5):1357-9.
- Madrigal E. Going remote: maintaining normalcy in our pathology laboratories during the COVID-19 pandemic. Cancer Cytopathol. 2020 May;128(5):321-2.
- Collier S. A geriatric psychiatry virtual rotation during Covid-19. Am J Geriatr Psychiatry. 2020 May [Epub ahead of print].
- Almarzooq ZI, Lopes M, Kochar A. Virtual learning during the COVID-19 pandemic: a disruptive technology in graduate medical education. J Am Coll Cardiol. 2020 May 26;75(20):2635-8.
- Chick RC, Clifton GT, Peace KM, et al. Using technology to maintain the education of residents during the COVID-19 pandemic. J Surg Educ. 2020 Jul-Aug;77(4):729-32.
- New England College of Optometry [Internet]. Boston: Alumni Magazine; c2020. Faculty create unique case-based clinical training; 2020 May 27 [cited 2020 June 16]; [about 2 screens]. Available from: https://www.neco.edu/news/entry/faculty-create-unique-case-based-clinical-training
- Hughes RG, editor. Patient safety and quality: an evidence-based handbook for nurses. Rockville (MD): Agency for Healthcare Research and Quality (US); 2008. Chapter 51, Enhancing patient safety in nursing education through patient simulation; 221-60 p.
- Aebersold M, Tschannen D. Simulation in nursing practice: the impact on patient care. Online J Issues Nurs. 2013 May;18(2):6.
- Liu C, Scott KM, Lim RL, Taylor S, Calvo RA. EQClinic: a platform for learning communication skills in clinical consultations. Med Educ Online. 2016 Jul;21:31801.
- Coleman D, McLaughlin D. Using simulated patients as a learning strategy to support undergraduate nurses to develop patient-teaching skills. Br J Nurs. 2019 Nov;28(20):1300-6.
- Pancholi B, Dunne MC. Virtual patient instruction and self-assessment accuracy in optometry students. Optometric Education. 2018;43(2):1-16.
- Morhardt T, McCormack K, Cardenas V, Zank J, Wolff M, Burrows H. Vaccine curriculum to engage vaccine-hesitant families: didactics and communication techniques with simulated patient encounter. MedEdPORTAL. 2016 May;12:10400.
- Sleight WE. Assessment of the ocular disease diagnostic tutor as a learning tool. Optometric Education. 2011;36(2):63-71.
- Scheiman M, Whittaker S. Implementing problem based learning in the didactic curriculum. Optometric Education. 1990;15(4):113-8.
- Puentedura RR. Hippasus: SAMR: moving from enhancement to transformation [Internet]. Williamstown (MA): Reuben Puentedura. 2013 May [cited 2020 Jun 16]. Available from: https://www.hippasus.com/rrpweblog/archives/2013/05/29/SAMREnhancementToTransformation.pdf
- Woodruff CE, Wagner H. Utilization of technology in optometric education: moving from enhancement to transformation. Optometric Education. 2019;44(2):7-13.
- Hamilton ER, Rosenberg JM, Akcaoglu M. The substitution augmentation modification redefinition (SAMR) model: a critical review and suggestions for its use. TechTrends. 2016 Sep;60(5):433-41.
- del Bueno D. A crisis in critical thinking. Nurs Educ Perspect. 2005 Sep-Oct;26(5):278-82.
- Denial A. The impact of the perceived value of critical-thinking skills. J Excell Coll Teach. 2012;23(1):69-97.
- Klenke-Borgmann L. High-fidelity simulation in the classroom for clinical judgment development in third-year baccalaureate nursing students. Nurs Educ Perspect. 2020 May-Jun;41(3):185-6.
- Myers A. Cognitive science insights for professions’ education. Optometric Education. 1990;15(4):105-10.
- Curran V, Matthews L, Fleet L, Simmons K, Gustafson DL, Wetsch L. A review of digital, social, and mobile technologies in health professional education. J Contin Educ Health Prof. 2017;37(3):195-206.
- Cheston CC, Flickinger TE, Chisolm MS. Social media use in medical education: a systematic review. Acad Med. 2013 Jun;88(6):893-901.
- Greenhow C, Lewin C. Social media and education: reconceptualizing the boundaries of formal and informal learning. Learn Media Technol. 2016;41(1):6-30.
- Stewart MA. Effective physician-patient communication and health outcomes: a review. CMAJ. 1995 May;152(9):1423-33.
- Kilgour JM, Grundy L, Monrouxe LV. A rapid review of the factors affecting healthcare students’ satisfaction with small-group, active learning methods. Teach Learn Med. 2016;28(1):15-25.




