Terrien’s Marginal Degeneration
Todd Peabody, OD, MBA, FAAO, Kelly Boucher, OD, Kimberly Cheney, OD
Abstract
Terrien’s marginal degeneration (TMD) is a rare disease with an unknown cause. This teaching case report highlights the presentation, differential diagnosis and management and treatment of TMD. It is intended to help eyecare providers recognize the condition and provide proper patient education and management.
Key Words: Terrien’s, cornea, ectasia, anterior segment
Background
Terrien’s marginal degeneration (TMD) is a rare, slowly progressive, peripheral corneal ectasia of unknown etiology. The condition is most commonly seen in males past the age of 40. Initially, TMD presents as small, yellow-white, stromal opacities composed of lipids with some superficial vascularization, which begins superiorly and spreads circumferentially. With progression, a gutter forms in the affected area due to stromal thinning, leaving the epithelium intact. The condition is often bilateral and asymmetric. Perforation of the cornea is rare but may occur spontaneously or secondary to trauma. Patients are often asymptomatic but may complain of mild irritation or vision changes due to increasing against-the-rule or oblique astigmatism.
This teaching case report is intended for optometry students at all levels. For first- and second-year students, emphasis can be on corneal structure and diagnostic testing that can be performed. For third- and fourth-year students and residents, the same concepts can be stressed, with the addition of differential diagnosis and treatment and management of patients with TMD.
Case Description

Figure 1. Stromal opacities in the superior cornea OD.
Click to enlarge
The patient, a 52-year-old Caucasian male, was seen at the clinic for a comprehensive ocular examination. He complained that his wife had noticed some coloration changes “on his right iris” in the upper quadrant. She noticed this “discoloration” about one month earlier. He reported no other problems such as eye pain, flashes, photophobia, diplopia, headaches or trauma. He did have longstanding floaters with no recent changes or increase in number. His last eye exam was approximately 10 years ago. The only significant ocular diagnosis at that examination was an alternating exotropia.
The patient’s medical history included a recent tooth abscess for which he underwent a root canal and finished a round of antibiotics. The eye discoloration was present before the round of antibiotics. His history also included occasional mild joint pain. His current medications and supplements included glucosamine, methylsulfonylmethane (MSM), fish oil and turmeric. His only reported allergy was to penicillin. The patient stated that he had never been a smoker, did not currently drink, and did not use any recreational drugs. Blood pressure was taken in-office from the right arm with the patient in a seated position and measured 120/78 mmHg. Weight and height were 175 lbs. and 67.5 in. BMI was calculated at 27. Family history included a paternal grandmother who had type 1 diabetes, a sister who had suffered a stroke, and a father who was hypertensive. The patient was oriented to time, place and person, and his mood and affect were appropriate.
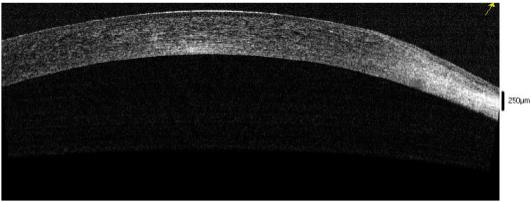
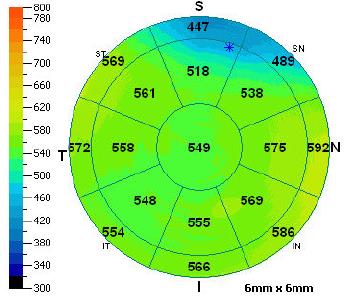 Figure 2A and 2B. Anterior segment OCT depicting superior nasal thinning OD. |
The patient’s entering visual acuities were OD 20/50- distance and 20/25- near, and OS 20/20- distance and 20/40 near. He did not present with glasses; therefore, all visual acuities were taken without correction. The patient’s pupils were equal, round and reactive to light and accommodation without afferent pupillary defects OD, OS. Extraocular muscles were full with no restrictions. FDT perimetry was full with no defects. Cover test confirmed an 18 prism diopter constant alternating exotropia at distance and near. Subjective refraction was OD -1.00 – 1.00 x 055, and OS -0.25 – 0.75 x 090. A +2.00 add resulted in visual acuities of 20/20 OD and OS at both distance and near.
Slit lamp examination revealed superior yellow-white stromal opacities extending circumferentially from 11 to 3 o’clock with superficial corneal limbal neovascularization OD. The left eye was unremarkable. Intraocular pressures as measured by Goldmann tonometry were 20 mmHg OD and 18 mmHg OS. Dilated fundus examination showed cup to disc ratios of 0.20 round OD and 0.25 round OS with no other ocular pathology.
Follow-up: one month after initial presentation
At a one-month follow-up visit, the condition appeared to be stable with no advancement. The patient was educated about the progressive nature of this condition and the importance of wearing eye protection. He will be monitored closely for further progression as well as involvement of the other eye.
Additional testing
Additional testing performed at the one-month follow-up included anterior segment photos that were taken using the slit lamp biomicroscope and an iPhone (Figure 1). Anterior
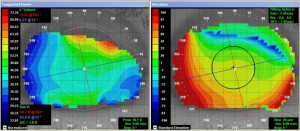
Figure 3. Corneal topography OD showing curvature change superiorly.
Click to Enlarge
segment optical coherence tomography (OCT) was also performed, and it showed thinning in the areas of the stromal opacities (Figure 2). Corneal topography was performed and revealed a change in curvature superiorly, in the areas of stromal opacity, consistent with thinning and flattening (Figure 3). Unfortunately, the topographical maps were not clear in the area of the superior cornea. Image acquisition proved challenging in this patient due to lid position. At future visits, manual attempts to better manage the lid position should be considered.
Learning Objectives
► to describe the ocular presentation of Terrien’s marginal degeneration
► to describe additional testing that can be performed to confirm a diagnosis
► to describe treatment and management for Terrien’s marginal degeneration
► to identify differentials that can mimic Terrien’s marginal degeneration
Key Concepts and Discussion Points
► Ocular anatomy
● corneal layers
● corneal histology
► Ancillary diagnostic tests
● placido topography
● scanning slit topography
● anterior segment optical coherence tomography
● ultrasound biomicroscopy
● in vivo confocal microscopy
► Ocular disease
● ocular findings
● differential diagnosis
• arcus senilis
• Mooren’s ulcer
• keratoconus
• pellucid marginal degeneration
• vernal keratoconjunctivitis
• ocular rosacea
► Patient education, treatment and management
Literature Review
Terrien’s marginal degeneration is a slowly progressive thinning of the peripheral cornea. It usually begins superior-nasally and progresses circumferentially. Yellow-white stromal opacities with superficial neovascularization are present. These stromal opacities are composed of scarring and lipid infiltration, and there is a distinct interval between the limbus and site of infiltration. Ultimately, stromal degeneration occurs, causing formation of a peripheral gutter.1 The exact etiology of TMD is unknown, but there is male predilection [3:1]. The condition usually appears in the third to fifth decade of life, but it can occur at any age.2 Both eyes are commonly affected, but presentation can be asymmetric.1
Histological changes have been noted in patients with TMD. The epithelium remains intact while the subepithelial area degenerates.3 Lopez and associates presented a case of TMD that required a cresent-shaped keratoplasty. They noted that light microscopy of a lamellar corneal button revealed a thickened epithelium, with an irregular Bowman’s layer. The anterior stroma was infiltrated with inflammatory cells including lymphocytes and some neutrophils. The adjacent conjunctiva was infiltrated with a few lymphocytes as well.1 More recently, Ceresara and associates wrote of a case of TMD without perforation; in vivo confocal microscopy of the cornea was used to better evaluate the microstructures of the cornea. Confocal images revealed a normal superficial epithelium, irregular Bowman’s layer, and deposits of nonhomogeneous hyper-reflective material (corresponding to the lipid deposition) at the basal epithelium and anterior stroma. Neovascularization was present at the level of the basal epithelium in the paralimbal cornea. They also reported inflammatory cell infiltration at the level of the adjacent paralimbal conjunctiva and peripheral basal epithelium.2 Ferrari and colleagues published the results of a study in which in vivo confocal microscopy revealed similar findings without the presence of inflammatory cells.4
Recent studies suggest the use of scanning slit topography to aid in the diagnosis and differentiation of TMD from other corneal thinning disorders. Scanning slit topography utilizes optical slits that scan along multiple points of the cornea. A video camera positioned at a 45-degree angle from the cornea captures reflections of the slits. This allows for measurements of the anterior and posterior cornea, as well as corneal pachymetry.5 Topography mapping and videokeratography are useful tools in monitoring corneal curvature, elevation and the amount of corneal astigmatism. They are beneficial when fitting rigid gas permeable contact lenses for these patients. Typically in TMD, corneal topography reveals flattening over the peripheral areas of thinning with steepening opposite to the mid-point of thinning, which results in against-the-rule or oblique astigmatism. Scanning slit topography can also be used to monitor the anterior and posterior surfaces with respect to the “best fit sphere” (float) and corneal thickness. In a reported case of unilateral TMD (no slit lamp biomicroscopy findings in the contralateral eye), scanning slit topography float data revealed anterior and posterior elevation in the contralateral eye. In this case, keratometric maps showed skewing of principal meridians and corneal steepening. These changes, while not classic topographic evidence of TMD, may suggest the need for close monitoring to watch for progression.6
Due to its high magnification and ability to depict the size and shape of structures in the anterior segment, ultrasound biomicroscopy (UBM) has also been shown to be useful for monitoring the cornea. UBM is able to quantify the thickness of the cornea and help to detect progression of disease. It can reveal subtle changes in the cornea, including changes in Bowman’s layer, Descemet’s membrane and stromal structure.7
Treatment and management of TMD are largely supportive because patients are often asymptomatic. In the case of mild adjacent conjunctival inflammation, topical steroids may be used sparingly. Steroids should be used cautiously because they can exacerbate corneal melt and increase thinning. Topical ocular lubricants can provide comfort. Monitoring patients for progression plays a significant role in the management process. As already discussed, corneal topography, anterior segment OCT, confocal microscopy, biomicroscopy and ultrasound biomicroscopy are all sound clinical options for following progression. Due to risk of corneal perforation in the area of TMD, polycarbonate lenses are highly recommended, as are American National Standards Institute-compliant safety glasses when warranted. If spectacle correction of vision is not possible due to complex or irregular astigmatic changes, piggybacked rigid gas permeable contact lenses or scleral lenses are both viable options. It is recommended that patients wear plano polycarbonate lenses over their contact lens prescription.
If corneal perforation occurs or if a patient is at high risk of perforation, a crescentic lamellar or full-thickness keratoplasty8,9 can be performed. A lamellar keratoplasty does not replace the entire thickness of the cornea. Instead, only Bowman’s layer and the anterior portion of the corneal stroma are replaced. Descemet’s membrane, the endothelium and the deep stroma are left intact. A crescentic lamellar keratoplasty utilizes this technique when only the thinned portion of the patient’s cornea is replaced with crescent-shaped donor cornea while the rest remains preserved. Lamellar keratoplasties are often preferred over penetrating keratoplasties because of the decreased risk of graft rejection, irregular astigmatism and corneal opacification. Symptoms of perforation can range from a decrease in visual acuity to tearing or pain. Signs of perforation include a positive Seidel sign, a shallow or flat anterior chamber, and folds in Descemet’s membrane. At the onset of clinical care for TMD, patients should always be informed of the possibility of perforation.10
Differential Diagnosis
It is important for the clinician to recognize and be able to differentiate Terrien’s marginal degeneration from other corneal pathologies that can have similar appearances, including arcus senilis, Mooren’s ulcer, keratoconus, pellucid marginal degeneration (PMD), vernal keratoconjunctivitis (VKC) and ocular rosacea.
► Arcus senilis is the most common peripheral corneal opacity. Stromal lipid deposits begin in the superior and inferior perilimbal cornea and progress circumferentially to form a band approximately 1 mm wide. The peripheral edge is sharp and separated from the limbus by a clear zone. The translucent interval may undergo mild thinning.10
► Mooren’s ulcer is a rare, idiopathic, circumferential stromal ulceration in the peripheral cornea. It can be unilateral or bilateral with no specific age demographic. Mooren’s ulcer is usually associated with moderate to severe pain, photophobia and blurred vision secondary to astigmatism. An autoimmune trigger or a history of insult or trauma to the cornea may be responsible for Mooren’s ulceration. Ulceration involves the anterior one-third of the cornea and progresses circumferentially and centrally with infiltration and vascularization at the leading edge.10
► Keratoconus is a progressive stromal thinning occurring centrally or paracentrally. It usually affects both eyes but can be asymmetric. Onset usually occurs around puberty. Signs of keratoconus include scissoring reflex on retinoscopy; slit lamp exam may reveal Vogt striae (vertical tension lines in the posterior cornea) and/or an epithelial Fleischer ring (epithelial iron deposits at the cone base). Keratoconus patients often have irregular astigmatism with steep keratometry readings. Munson’s sign, which is bulging of the lower eyelid on down-gaze, may also be present. In severe cases, acute hydrops (stromal edema due to leakage of aqueous humor through a tear in Descemet’s membrane) may occur.10
► PMD is a rare thinning of the inferior cornea that causes reduced visual acuity. It is usually bilateral but can be asymmetric. Onset occurs during the fourth and fifth decades of life. Clinical presentation is a slowly progressive band of inferior thinning extending down to 1 mm from the limbus. Unlike in keratoconus, there is no Fleischer ring or Vogt striae, and PMD presents with an area of steepening superior to the area of corneal thinning.10
► VKC is a recurrent bilateral disorder. It primarily affects young boys around the age of 7. VKC is more common in warmer, dry areas such as the Mediterranean, sub-Saharan Africa and Middle East. Symptoms include itching, photophobia, foreign body sensation and mucous discharge. VKC can affect the limbal area of the cornea, the palpebral conjunctiva, or both. Signs include giant papillae on the superior tarsal conjunctiva and/or limbal papillae with or without a white apex called Horner-Trantas dots. Corneal changes such as punctate epithelial erosions, macroerosions and shield ulcers can also occur.10
► Ocular rosacea affects 6-18% of patients with systemic rosacea. Rosacea is an idiopathic skin condition affecting sun-exposed areas. Clinical features range from facial flushing to a papulopustular rash and, in later stages, thickening of the skin that can evolve into rhinophyma. Ocular symptoms include irritation, burning and tearing. The lids, conjunctiva and cornea can all be involved. The lids can show superficial telangiectasias and blepharitis. Conjunctival bulbar hyperemia may be present. The cornea can be impacted by minor punctate epithelial erosions, marginal keratitis and, in severe cases, corneal scarring and vascularization.10
Discussion
Although Terrien’s marginal degeneration is rare, it is important that eycare providers differentiate it from other conditions so they can set patient expectations and initiate proper management and treatment. A thorough case history and careful slit lamp examination are essential. It is imperative to use topical steroids conservatively due to the risk of corneal thinning. Corneal perforation is rare with TMD, but early prescription of polycarbonate lenses can reduce the risk by offering protection from blunt trauma.
Conclusion
This case report is intended to educate eyecare providers on the presentation and management of Terrien’s marginal degeneration. It reviews multiple ways to monitor the progression of the disease, as well as treatment options depending on the severity of thinning. This case report points out the distinguishing characteristics of TMD and other differentials. This information should be helpful to eyecare providers when they encounter a rare case of TMD.
References
1. Lopez JS, Price FW, Whitcup SM, et al. Immunohistorychemistry of Terrien’s and Mooren’s corneal degeneration. Archives of Ophthalmology. 1991;109(7):988-992.
2. Ceresara G, Migliavacca L, Orzalesi N, Rossetti L. In vivo confocal microscopy in Terrien marginal corneal degeneration: a case report. Cornea. 2011;30(7):820-824.
3. Guyer DR, Barraquer J, McDonnell PJ, Green WR. Terrien’s marginal degeneration: clinicopathologic case reports. Graefes Archive Ophthalmology 1987;225(1):19-27.
4. Ferrari G, Tedesco S, Delfini E, Macaluso C. Laser scanning in vivo confocal microscopy in a case of Terrien marginal degeneration. Cornea. 2010;29(4):471-475.
5. Review of Cornea and Contact Lenses [Internet]. Yeung KK, Chang S. New equipment sees the cornea better. c2011 [cited 2015 July 17] Available from https://www.reviewofcontactlenses.com/content/d/disease/c/30278/.
6. Fernandes M. Scanning slit topography: Diagnostic boon in presumed unilateral Terrien’s marginal degeneration. Cont Lens Anterior Eye. 2011;34(6):282-286.
7. Skribek A, Sohár N, Gyetvai T, Nógrádi A, Kolozsvári L. Role of ultrasound biomicroscopy in diagnosis and treatment of Terrien disease. Cornea. 2008;27(4):427-433.
8. Eyenet [Internet] Vishak J, Goins KM, Afshari NA. Deep anterior lamellar keratoplasty. c2007 [cited 2015 July 17] Available from https://www.aao.org/publications/eyenet/200709/pearls.cfm.
9. Cheng CL, Theng JT, Tan DT. Compressive C-shaped lamellar keratoplasty: a surgical alternative for the management of severe astigmatism from peripheral corneal degeneration. Ophthalmology. 2005;112(3):425-430.
10. Kanski J, Bowling B, Nischal K. Clinical ophthalmology: a systematic approach (7th ed.). Edinburgh: Elsevier/Saunders; 2011.