PEER REVIEWED
Hydroxychloroquine Retinal Toxicity
Stanley Tang, OD, FAAO, and Angelina Tran, OD, FAAO
Abstract
Hydroxychloroquine (Plaquenil) is a common medication used in the management of rheumatologic conditions and malaria. Ocular toxicity is a possible side effect of hydroxychloroquine usage. This case report outlines a patient presenting for hydroxychloroquine screening with toxicity observed on visual field testing and optical coherence tomography of the macula. Continual progression of his visual field damage was observed after discontinuation of the medication at our recommendation. A review of historic and current hydroxychloroquine screening guidelines is included in this report.
Key Words: hydroxychloroquine, Plaquenil, maculopathy, visual field, multifocal ERG, optical coherence tomography
Background
Hydroxychloroquine (Plaquenil, Novartis, East Hanover, N.J.) is a drug initially developed in the mid-1950s for management of malaria and is a derivative of chloroquine. The hydroxylation of chloroquine has resulted in a decreased incidence of side effects while maintaining efficacy.1 Currently, hydroxychloroquine is used for management of various rheumatologic conditions, including rheumatoid arthritis, systemic lupus erythematosus, and Sjogren’s syndrome. In the future, hydroxychloroquine may also be used in the management of other medical conditions. Early studies show promising results in the control of hemoglobin A1c (HbA1c) levels for individuals with diabetes.2,3 There is also anecdotal evidence suggesting hydroxychloroquine (used concurrently with azithromycin) may be an effective treatment for coronavirus disease 2019 (COVID-19) infections caused by the coronavirus initially discovered in late 2019.4
Hydroxychloroquine has been observed to cause significant ocular side effects, including retinal toxicity and, less commonly, anterior segment changes.5 Symptoms include reduced vision, paracentral scotoma, photopsia and glare. The American Academy of Ophthalmology (AAO) released updated guidelines in 2016 for screening protocols for individuals who have been prescribed hydroxychloroquine.12 Early detection of ocular toxicity is of utmost importance as retinal toxicity changes are irreversible and may continue to progress after discontinuation of the medication.
The following case report describes a 66-year-old White male who was diagnosed with retinal toxicity from hydroxychloroquine based on Humphrey visual field (HVF) 10-2 testing and macular optical coherence tomography (OCT) imaging. He subsequently discontinued hydroxychloroquine after consultation with rheumatology and was followed for progression of visual field damage.
Case Report
A 66-year-old Caucasian male presented as a new patient for his annual comprehensive eye exam. He had a history of hydroxychloroquine use for management of discoid lupus. His dosage was 200 mg orally BID, with a total daily dose of 400 mg. He had been followed previously by another eyecare provider but was lost to follow-up for four years. His total duration of dosing of hydroxychloroquine was approximately seven years.
The patient’s medical history included discoid lupus, irritable bowel syndrome, hypertension and chronic obstructive pulmonary disease. There was a noted lack of renal impairment in the patient’s medical history. His daily medications included hydroxychloroquine, amlodipine, hydrochlorothiazide and albuterol inhaler. He had no prior history of ocular trauma or surgery. His previous ocular health record from four years prior included cataracts and a choroidal nevus in the left eye, with no mention of maculopathy in either eye.
Entering uncorrected visual acuities were 20/30 OD and 20/30-2 OS. His best-corrected visual acuities after manifest refraction were 20/20 OD and 20/20 OS, with low astigmatic correction in both eyes. Pupil reactivity, confrontation visual fields and ocular motility were normal in both eyes. Intraocular pressure measured 18 mmHg OD and 17 mmHg OS with Goldmann applanation tonometry.
Slit lamp examination of the anterior segment was unremarkable in both eyes, including a noted absence of corneal deposits in both eyes. Dilated posterior segment examination revealed mild nuclear sclerotic changes of the lens in both eyes. The vitreous was clear in both eyes. The patient’s optic nerve cup-to-disc ratio was 0.30H/0.35V OD and 0.35H/0.35V OS. His maculae were flat and evenly pigmented without obvious presence of bull’s eye maculopathy or macular pigmentary disruption. The posterior pole in the left eye exhibited a flat choroidal nevus 1 disc-diameter in size along the superior arcade with overlying drusen and no observable lipofuscin. The peripheral retina was unremarkable in both eyes.
HVF 10-2 testing, performed prior to his dilated exam, revealed an early-to-moderate paracentral ring scotoma with sparing of the central two degrees in the right eye. The left eye visual field test revealed an early paracentral ring scotoma, also with sparing of the central two degrees (Figure 1). This was a significant change from his baseline visual field testing from four years ago, which was reliable and without evidence of a paracentral scotoma (Figure 2).
Baseline spectral-domain OCT (SDOCT, Heidelberg Spectralis) of the macula revealed subtle thinning of the outer nuclear layer of the right eye and normal macular appearance in the left eye. Ellipsoid zone disruption was present in both eyes (Figure 3). The image captured was a 25-line horizontal raster scan.
The patient was educated on his diagnosis and advised to return in three months for repeat HVF 10-2 testing to monitor for further progression of the visual field loss. The patient’s rheumatologist was notified of the findings of early retinal toxicity and he discontinued the use of hydroxychloroquine immediately.
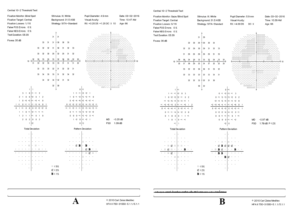 Figure 1. Humphrey visual field 10-2 results for left eye (A) and right eye (B). Note the paracentral ring scotoma in the right more than left eye, with sparing of the central two degrees. |
 Figure 2. Baseline Humphrey visual field 10-2 results for the left eye (A) and right eye (B) from historical record review. |
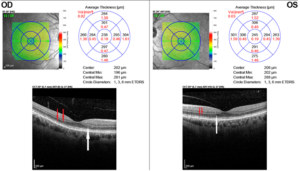 Figure 3. Macular optical coherence tomography results indicating subtle inner segment/outer segment (IS/OS) junction disruption (red arrows) and thinning of the outer nuclear layer just nasal to the fovea in the right eye (white arrow). There is mild IS/OS junction disruption (red arrows) and outer nuclear thinning in the left eye (white arrow). Click to enlarge |
 Figure 4.Progression of the patient’s visual field 10-2 results in both eyes. Note the progression of the visual field damage despite discontinuation of hydroxychloroquine. However, the field appears stable starting at seven months after discontinuation. |
The patient had repeat HVF 10-2 testing performed two months, six months and approximately 18 months later (Figure 4). There was continual progression of visual field loss after discontinuation of hydroxychloroquine for approximately six months. The patient has been followed on an annual basis, and his visual field appeared stable at his most recent examination, 18 months post-discontinuation.
Educator’s Guidelines
Key concepts
- Overview of current AAO screening guidelines
- Understanding high-risk characteristics and risk factors for hydroxychloroquine toxicity
- Detection and observation of early ancillary testing changes associated with hydroxychloroquine toxicity
Learning objectives
At the conclusion of this case discussion, participants should be able to:
- Review a patient’s ocular and medical history to determine risk factors for retinal toxicity
- Understand risk factors and tailoring of hydroxychloroquine screening guidelines based on individual patient medical history
- Observe early changes in HVF, OCT, fundus autofluorescence (FAF) and multifocal electroretinography (mfERG) test results for early detection
- Co-manage individuals taking hydroxychloroquine with rheumatology
- Be familiar with future directions of hydroxychloroquine use outside of rheumatologic disorders
Discussion questions
1. Knowledge and concepts required for critical review of the case
- What are current AAO screening guidelines for when to initiate annual screening?
- Which risk factors have the greatest impact on development of retinal toxicity?
- How does early retinal toxicity manifest in HVF, OCT, FAF and mfERG?
2. Differential diagnoses
- What are likely differential diagnoses to be considered for this case?
- When is ancillary testing recommended?
- What additional testing can be done to differentiate hydroxychloroquine toxicity from other differential diagnoses considered above?
3. Disease management
- What management would you recommend to this patient or similar patients?
- How often would you follow this patient after diagnosis of toxicity?
- Are there any at-home tests or other methods for these patients to monitor for changes?
4. Patient education
- What would you tell the patient about the prognosis of this condition?
- How would you discuss systemic risk factors that may relate to retinal toxicity?
- How would you educate this patient to understand continued follow-up with rheumatology is necessary?
5. Critical thinking
- Would you have done anything differently in management of this case? Please elaborate.
- Would your screening of this patient vary if he were a different race? If so, what would you change?
Discussion
Teaching instructions
This case report targets third- and fourth-year optometry students and optometry residents. Prior knowledge of visual field testing and observation of retinal layers on OCT are expected. Readers should study the entire background and case report, including OCT scans and visual field test results, and answer all discussion questions in the Education Guidelines section. The questions will guide assessment in the success of learning objectives. This case will likely be best presented as a PowerPoint presentation due to its graphical nature and need for interpretation of ancillary testing. In addition, a combination of PowerPoint and verbal case discussion will best convey background concepts within this teaching case report.
Background
Hydroxychloroquine is a chloroquine derivative originally developed for management of malaria. Although it has limited use as an anti-malarial due to development of chloroquine-resistant strains of malaria, historical experimentation during the early to mid-1950s led to the discovery of its anti-inflammatory properties.1 It has since been used for management of rheumatoid arthritis, systemic lupus erythematosus and other rheumatic conditions.1
Hydroxychloroquine may also be useful in the management of diabetes as an alternative to traditional diabetic medications.2,3 Hsia et al. reviewed diabetic management in patients taking the maximum dose of metformin and a sulfonylurea. 400-mg dosing of hydroxychloroquine was compared with 45 mg pioglitazone as third-line drugs for diabetic management. After a two-month clinical trial, the authors noted a decrease in HbA1c levels of 1.2% for patients in the hydroxychloroquine group, and a 2.8% decrease in HbA1c levels for patients in the pioglitazone group. The authors noted cost efficiency should be considered, as hydroxychloroquine is available for substantially lower cost than pioglitazone.3
The global COVID-19 pandemic shined a new light on hydroxychloroquine (combined with azithromycin) as a potential treatment for the symptoms caused by COVID-19.7 Although studies have produced mixed results and are limited in size and scope, some evidence has been found to suggest hydroxychloroquine, when combined with azithromycin, may decrease viral load of the novel coronavirus.7 Gautret et al. observed in a small study that 600 mg of hydroxychloroquine daily, combined with azithromycin, led to a significant reduction in viral load after six days of treatment.8 All six patients treated with combined azithromycin and hydroxychloroquine showed a negative nasopharyngeal polymerase chain reaction test at day six. This is in contrast with using hydroxychloroquine alone, which led to eight of 14 patients testing negative after six days.8 As COVID-19 is an ever-changing public health crisis, further studies indicated limited justification for the use of hydroxychloroquine for management of the virus. This ongoing debate centered around hydroxychloroquine led to shortages in supply of the drug, causing concern for both rheumatologists and patients.9 A more recent study by Geleris and Sun followed 1,376 patients, with 58.9% receiving hydroxychloroquine. Patients receiving hydroxychloroquine were dosed at 600 mg BID on day one, then 400 mg daily for an additional four days. Respiratory failure developed in 25.1% of patients studied, which the authors defined as the primary endpoint for their study. The authors stated there was no significant association between hydroxychloroquine use and the primary endpoint.10 The risk of respiratory failure or death was not significantly higher or lower among those who were administered hydroxychloroquine according to the regimen above, contradicting the prior smaller-scale European study.10
Individuals who have been prescribed hydroxychloroquine are at risk to develop both anterior and posterior segment ocular side effects.5 Although rare, corneal epithelial deposition is possible and generally occurs within the inferior cornea.5,6 Grierson noted an overall incidence of keratopathy of 0.8% (six cases of 758 patients studied).6 However, in four of these cases, the dosing was greater than 6.5mg/kg daily.6 These corneal deposits are typically not visually significant and are reversible upon discontinuation of therapy.5,6 Cataract and accommodative dysfunction have been found to occur in patients taking chloroquine; however, these side effects have not been observed in individuals prescribed hydroxychloroquine.19
Retinal toxicity can have devastating visual consequences if not detected early. Current guidelines released by the AAO in 2016 include a few changes from the previous revision in 2011.12 The AAO accumulated significant data from 2,361 patients who were prescribed hydroxychloroquine for more than five years. The authors noted an overall 7.5% prevalence of hydroxychloroquine retinopathy. Incremental risk for an individual using ≤ 5.0 mg/kg daily dosing is less than 1% during the first 10 years of use. This increases to 4% after 20 years. However, it can reach an approximate risk of 20% after 20 years of use with higher dosing.16 Current AAO guidelines state that annual screenings are recommended after five years of use. Marmor et al. noted that patients prescribed hydroxychloroquine at ≤ 5.0 mg/kg daily for less than five years have less than 1% risk of developing retinal toxicity.12
The daily dose recommendation of hydroxychloroquine has changed from < 400 mg daily in 2011 to < 5mg/kg daily.12 The historical 400-mg daily dosing calculation was calculated from a patient’s ideal body weight (IBW) and recommendations of hydroxychloroquine dosing to be 6.5 mg/kg IBW. However, Walvick et al. noted that dosing through IBW led to 56% of females and 46% of males receiving higher than the recommended dose of hydroxychloroquine.13 Marmor et al. also determined that there is a stratification of risk based on actual body weight (ABW) dosing of hydroxychloroquine: 5mg/kg daily dosing ABW led to two to three times greater risk of developing hydroxychloroquine retinopathy compared with 4-mg/kg daily dosing ABW.12
The cumulative dosing guideline of > 1,000 g total dose established in 2011 has been removed. A total cumulative dose of 1,000 g can be established through 400-mg daily dosing for 6.85 years, or 200-mg daily dosing for 13.7 years.16 Because the AAO already recommends screening after five years, this guideline is no longer thought to be relevant.
Systemic risk factors for hydroxychloroquine retinal toxicity include renal impairment and current tamoxifen use. Renal impairment has been associated with higher serum hydroxychloroquine concentration, as hydroxychloroquine is excreted through the renal system.14 Melles and Marmor stated that a 50% reduction in glomerular filtration rate is associated with doubling of hydroxychloroquine retinopathy risk.15 Also, it should be noted that although hydroxychloroquine is partially metabolized within the liver, the authors found no increase in risk of hydroxychloroquine retinopathy for individuals with documented liver disease.12,24 Tamoxifen, commonly used in the management of breast cancer, is now noted as a significant risk factor for development of retinopathy when taken concomitantly with hydroxychloroquine; there is an up-to-five-fold increased risk of development of retinopathy when the two are taken in combination.12 Although the underlying physiology of this increased risk is not known, it is speculated that the two drugs have an adverse metabolic synergistic effect.12 This is another major change from the AAO 2011 guidelines to its 2016 revision.
Upon encountering a patient with current hydroxychloroquine usage, it is imperative to ask specific questions about his/her medical and ocular history to determine the risk of retinal toxicity. As outlined above, one should confirm the patient’s dosing and duration of use and inquire about an estimated weight. This will allow for calculation of the ABW dosing, which can be used to determine whether a patient is taking a high-risk or low-risk dose of hydroxychloroquine. In addition, a careful review of medications and patient medical history (including presence or absence of renal disease) should be performed to determine risk of toxicity.
Currently, baseline examination is recommended within the first year of initiating hydroxychloroquine and annually after five years of use. In addition, the drug manufacturers also recommend baseline examination prior to starting therapy to rule out pre-existing maculopathies.16 The current AAO guidelines also state that pre-existing maculopathy is a risk factor for development of hydroxychloroquine retinopathy; however, Yusuf et al. found no data to suggest pre-existing maculopathy leads to increased susceptibility of hydroxychloroquine retinopathy.16 Patients with minimal baseline macular abnormality, including mild macular drusen, should not be excluded from therapy.16 However, pre-existing macular conditions may interfere with interpretation of ancillary testing and detection of early toxic retinopathy. Major macular pathology is a contraindication to hydroxychloroquine use.16
Diagnosis and clinical findings
Diagnosis of early-stage hydroxychloroquine retinopathy largely relies on ancillary testing, including HVF 10-2 and 24-2, macular OCT, FAF and mfERG. AAO guidelines state that the recommended tests are HVF 10-2 and SDOCT; FAF and mfERG are noted as discretionary.16 Of note, the 2016 guidelines recommend HVF 24-2 and widefield SDOCT testing for patients of Asian descent as these patients tend to exhibit extramacular toxicity.14
Toxicity detected through HVF 10-2 testing is typically observed as a paracentral ring scotoma, normally from two to six degrees of fixation, with sparing of the central two degrees.27 Particular attention should be given in the superior nasal region as the inferior temporal retina tends to be affected early.20 A low threshold for suspicion is important in early diagnosis; defects may initially be discounted as non-specific scatter due to the subjective nature of visual field testing. In addition, patients of Asian descent may have visual field loss beyond eight degrees from the fovea.18 It should also be noted that central defects found on HVF 24-2 testing warrant further testing with the 10-2 test strategy. A single-point depression centrally in the HVF 24-2 testing strategy may be a significant central loss on HVF 10-2 testing.27 In this clinical case, Figures 2A and 2B show an early paracentral defect that notably is sparing the central two degrees from fixation. The defect also appears to be limited to no further than six degrees from fixation. The characteristic pattern of visual field defect in the case outlined above was concerning for possible hydroxychloroquine toxicity.

Figure 5. Example of outer nuclear layer thinning noted within the white box. Compare outer nuclear layer nasally vs. laterally in the same image.
Click to enlarge
OCT is another essential tool for diagnosing maculopathy. It provides objective, detailed measurements of retinal structure. SDOCT testing is preferred over time-domain OCT, as the latter does not provide adequate resolution.12 Loss within macular OCT testing may be subtle on interpretation and requires careful attention. Disruption of the ellipsoid zone (also known as the inner segment/outer segment junction or the photoreceptor integrity line) may be observed in early stages of disease.26 Paracentral outer nuclear layer loss presents in moderate-stage disease; disruption and loss of the external limiting membrane may be observed as well.23 Figure 5 highlights an example of outer nuclear layer thinning on SDOCT (Heidelberg Spectralis) macular imaging. For the clinical case outlined here, Figures 3A and 3B show a disruption of the outer nuclear layer as well as the ellipsoid zone in both eyes on SDOCT (Heidelberg Spectralis) testing. The appearance of the SDOCT scan, in conjunction with the visual field findings noted above, were of concern for hydroxychloroquine toxicity.
OCT may also provide additional benefit due to widefield imaging capabilities that are now emerging in clinical care settings. Widefield imaging is beneficial for Asian patients who may develop extramacular toxicity.18,20,22 Choudhry et al. defined widefield imaging as up to a 50-degree field of view, with ultra-widefield imaging described as a 200-degree field of view in a single image.17 A study by Lee et al. reported that in eight out of nine patients with diagnosed retinal toxicity in a Korean population, the appearance was pericentral as opposed to the classic parafoveal.18 Particular attention is needed with observation of the inferior temporal retina as this area tends to be where early toxicity is first observed.16
FAF is another useful tool in evaluation of hydroxychloroquine retinopathy. Early toxicity may present itself as subtle paracentral hyperautofluorescence (or along arcades for Asians), with later stages appearing as hypoautofluorescence centrally surrounded by areas of hyperautofluorescence.19 Ahn et al. demonstrated observation of extramacular hydroxychloroquine retinopathy through widefield FAF in 70.7% of eyes examined in a Korean population.20 Imaging systems by Optos are able to achieve a field of view up to 200 degrees (Optos, Optomap Ultra-Widefield). Heidelberg also has developed widefield imaging techniques, which can provide a 105-degree field of view using a lens modification to the Heidelberg Retinal Angiograph.21
mfERG is considered the gold standard for hydroxychloroquine retinopathy screening as it may possibly detect toxicity earlier than other testing methods.22 The test produces a topographic map of ERG responses across the posterior pole. Reduced paracentral retinal responses are indicative of hydroxychloroquine toxicity.
Eyecare practitioners should recognize the importance of multiple modalities in confirming a diagnosis of hydroxychloroquine retinopathy. Greenstein et al. noted that functional changes in hydroxychloroquine retinopathy patients may be observed even before structural changes exist. Although OCT is a significant diagnostic tool, approximately half of patients with diagnosed toxicity in one study had normal SDOCT findings in the presence of abnormal HVF 10-2 and mfERG findings.23 In another study, Marmor and Melles observed 10% of patients examined with hydroxychloroquine toxicity showed a significant paracentral scotoma in absence of SDOCT abnormalities.19 Not only does this suggest that functional changes may present before structural changes, this also highlights the importance of using multiple ancillary tests to screen for hydroxychloroquine toxicity.
Patients may inquire about any possible at-home tests that may help them determine new presence of toxicity. Historically, the Amsler grid was thought to be a viable screening tool in hydroxychloroquine toxicity. However, the current AAO screening guidelines (2016 revision) list Amsler grid as not recommended for screening. Currently, there are no tests that can be done at home to screen for retinal toxicity.
Differential diagnosis
The differential diagnoses for hydroxychloroquine retinopathy include:
- Age-related macular degeneration (ARMD). Risk factors for ARMD include increased age, family history and personal history of smoking. Changes observed on macular OCT include central macular drusen and possibly intraretinal and/or subretinal fluid in cases of exudative macular degeneration. Symptoms include reduced vision, metamorphopsia, and central scotoma. The characteristic presence of drusen may be used to differentiate the two conditions.
- Cone or cone/rod dystrophy. Cone or cone/rod dystrophy is a result of congenital mutations in more than 30 genes, inherited through autosomal recessive patterns. These are typically diagnosed at a young age through genetic testing. Patients present with reduced vision, reduced color vision, central scotoma and peripheral vision loss. Peripheral vision loss is not typical of hydroxychloroquine retinopathy.
- Stargardt’s disease. Stargardt’s is a form of macular degeneration typically affecting children and young adults. Like cone/rod dystrophies, Stargardt’s is an inherited condition leading to reduced visual acuity, color vision and development of central scotoma. Diagnosis can be made through observation, ERG testing or genetic testing. One can differentiate Stargardt’s disease from hydroxychloroquine retinopathy due to age because Stargardt’s disease tends to affect a younger age cohort.
Management and prognosis
Currently, no treatment exists for hydroxychloroquine retinopathy, highlighting the significance of early diagnosis and communication with rheumatology. Retinal toxicity may be limited with early diagnosis, which is important as progression of visual field loss has been noted for years after discontinuation of therapy. Careful follow-up is necessary to continually monitor for changes in visual acuity and visual field. According to AAO screening guidelines, HVF 10-2 (or 24-2 in Asian patients) and OCT macular testing are used in diagnosis of hydroxychloroquine retinopathy.12 For individuals with suspected toxicity who are physically unable to perform HVF testing, referral to tertiary care centers or educational institutions with access to mfERG or FAF may be indicated. Table 1 highlights the newest guidelines for hydroxychloroquine screening.

Table 1. Click to enlarge
Upon diagnosis of retinal toxicity, eyecare providers should be in contact with rheumatology regarding the evidence of toxicity and recommendations to discontinue therapy. A balance of vigilance and understanding of expected functional and structural changes is needed to avoid premature discontinuation of therapy.
As noted by Marmor et al., the progression of structural changes on SDOCT depends on the stage of toxicity when diagnosed (and thus, how quickly hydroxychloroquine is discontinued). The authors stated that cases of early hydroxychloroquine toxicity showed little to no foveal structure changes measured on the Cirrus ETDRS cube. In contrast, individuals with moderate toxicity at time of diagnosis had progressive foveal thinning for at least three years. Severe toxicity at time of discontinuation had the most prominent progression of foveal thinning during this time frame. The authors defined early toxicity as “patchy damage within the parafoveal zone shown by field or objective testing.” Moderate toxicity was defined as “50% to 100% parafoveal ring of damage and marked thinning of the parafoveal retina on SDOCT without retinal pigment epithelium (RPE) damage.” Severe toxicity was defined as “bull’s-eye damage with RPE involvement on SDOCT (visible retinopathy).”26
The authors also noted the ellipsoid zone, which needs to maintain structural integrity for preservation of visual acuity, is left intact after three years in cases of early and moderate toxicity. This further highlights the importance of early detection in preservation of visual acuity, as severe toxicity showed progressive loss of the foveal ellipsoid zone.23
Patients should be aware of their hydroxychloroquine screening results and prognosis should any presence of toxicity occur. It is imperative to highlight the importance of retinal toxicity screening and advise them that early discontinuation of therapy is necessary to limit the continual progression of visual field defects. Patients should also be educated about the risk of continual progression of visual field changes even years after discontinuation. Several risk factors, such as renal impairment, tamoxifen use and > 5mg/kg daily dosing are associated with an increased risk of retinal toxicity development. Therefore, changes to a patient’s medical history should be reported to the eyecare practitioner so modifications can be considered to the screening regimen. Follow-up with rheumatology is also important because rheumatologic symptoms may worsen after discontinuation of hydroxychloroquine.
Conclusion
The case presented demonstrates important concepts related to careful evaluation and review of patient medical history, detection and communication in relation to hydroxychloroquine retinal toxicity. Optometrists play a crucial role in screening and detection related to hydroxychloroquine, which remains one of the most commonly prescribed drugs for rheumatologic conditions today. Individual medical history must be reviewed in great detail, as factors such as medication use and renal disease may greatly increase the risk of toxicity. Optometrists must be aware of both a patient’s hydroxychloroquine dosing and ABW to determine his or her risk of retinal toxicity through calculation of mg/kg daily dosing. The authors of this teaching case report choose to screen prior to five years of use for individuals who have documented renal impairment, tamoxifen use or sustained dosing of > 5mg/kg daily. In addition, one may consider screening sooner than five years for patient peace of mind. Both objective and subjective ancillary testing is recommended, and thorough evaluation of results is paramount in early detection because progressive visual field loss can occur for years even after discontinuation of the medication. Early-stage toxicity may cause no visual symptoms, but late-stage toxicity may have devastating visual consequences.
References
- Bergman M. The Nine Lives of Hydroxychloroquine [Internet]. Dallas: RheumNow; c2015 [cited 2020 Sep 28]. Available from: https://rheumnow.com/blog/nine-lives-hydroxychloroquine.
- Chen YM, Lin CH, Lan TH, et al. Hydroxychloroquine reduces risk of incident diabetes mellitus in lupus patients in a dose-dependent manner: a population-based cohort study. Rheumatology (Oxford). 2015 Jul;54(7):1244-9.
- Hsia S, Duran P, Lee M, Davidson MB. Randomized controlled trial comparing hydroxychloroquine with pioglitazone as third-line agents in type 2 diabetic patients failing metformin plus a sulfonylurea: a pilot study. J Diabetes. 2020 Jan;12(1):91-4.
- Scuccimarri R, Sutton E, Fitzcharles M. Hydroxychloroquine: a potential ethical dilemma for rheumatologists during the COVID-19 pandemic. J Rheum. 2020 Jun 1;47(6):783-6.
- Yam J, Kwok A. Ocular toxicity of hydroxychloroquine. Hong Kong Med J. 2006 Aug;12(4):294-304.
- Grierson D. Hydroxychloroquine and visual screening in a rheumatology outpatient clinic. Ann Rheum Dis. 1997 Jan;56(3):188-90.
- Agrawal S, Goel AD, Gupta N. Emerging prophylaxis strategies against COVID-19. Monaldi Arch Chest Dis. 2020 Mar 30;90(1).
- Gautret P, Lagier J, Parola P, et al. Hydroxychloroquine and azithromycin as a treatment of COVID-19: results of an open-label non-randomized clinical trial. Int J Antimicrob Agents. 2020 Jul;56(1):105949.
- Yazdany J, Kim A. Use of hydroxychloroquine and chloroquine during the COVID-19 pandemic: what every clinician should know. Ann Intern Med. 2020 Mar;172(11):754-5.
- Geleris J, Sun Y, Platt J, et al. Observational study of hydroxychloroquine in hospitalized patients with Covid-19. New Eng J Med. 2020 Jun 18;382(25):2411-2418.
- Rynes RI. Ophthalmologic safety of long-term hydroxychloroquine sulfate treatment. Am J Med 1983 Jul;75(1A):35-9.
- Marmor MF, Kellner U, Lai TYY, Melles R,B Mieler WF. Recommendations on screening for chloroquine and hydroxychloroquine retinopathy (2016 revision). Ophthalmology. 2016 Jun;123(6):1386-94.
- Walvick MD, Walvick MP, Tongson E, Ngo CH. Hydroxychloroquine: lean body weight dosing. Ophthalmology. 2011 Oct;118(10):2100.
- Paperis K, Al-Charakh M, Nzuonkwelle S, McPherson M, Al-Marzooq A, Bhattarai B. Characteristics and outcomes among patients with autoimmune rheumatic diseases requiring a higher level of care. J Clin Rheum. 2020 Feb 12. Advance online publication: https://doi.org/10.1097/rhu.0000000000001321.
- Melles RB, Marmor MF. The risk of toxic retinopathy in patients on long-term hydroxychloroquine therapy. JAMA Ophthalmol. 2014 Dec;132(12):1453-60.
- Yusuf IH, Sharma S, Luqmani R, Downes SM. Hydroxychloroquine retinopathy. Eye. 2017 Jun;31(6):828-45.
- Choudhry N, Golding J, Manry MW, Rao RC. Ultra-widefield steering-based spectral-domain optical coherence tomography imaging of the retinal periphery. Ophthalmology. 2016 Jun;123(6):1368-74.
- Lee DH, Melles RB, Joe SG, et al. Pericentral hydroxychloroquine retinopathy in Korean patients. Ophthalmology. 2015 Jun;122(6):1252-6.
- Marmor MF. Comparison of screening procedures in hydroxychloroquine toxicity. Arch Ophthalmol. 2012 Apr;130(4):461-9.
- Ahn SJ, Joung J, Lee BR. Evaluation of hydroxychloroquine retinopathy using ultra-widefield fundus autofluorescence: peripheral findings in the retinopathy. Am J Ophthalmol. 2020 Jan;209:35-44.
- Yung M, Klufas MA, Sarraf D. Clinical applications of fundus autofluorescence in retinal disease. Int J Ret Vit. 2016 Apr 8;2:12.
- Tsang AC, Pirshahid SA, Virgili G, Gottleib CC, Hamilton J, Coupland SG. Hydroxychloroquine and chloroquine retinopathy: a systematic review evaluating the multifocal electroretinogram as a screening test. Ophthalmology. 2015 Jun;122(6):1239-51.
- Greenstein VC, Amaro-Quireza L, Abraham ES, Ramachandran R, Tsang SH, Hood DC. A comparison of structural and functional changes in patients screened for hydroxychloroquine retinopathy. Doc Ophthalmol. 2014 Dec 12;130(1):13-23.
- Marmor MF, Melles R.B Disparity between visual fields and optical coherence tomography in hydroxychloroquine retinopathy. Ophthalmology. 2014 Jun;121(6):1257-62.
- Korah S., Kuriakose T. Optical coherence tomography in a patient with chloroquine-induced maculopathy. Indian J Ophthalmol. Nov-Dec 2008;56(6):511-3.
- Marmor MF, Hu J. Effect of disease stage on progression of hydroxychloroquine retinopathy. JAMA Ophthalmol. 2014;132(9):1105-12.
- Anderson C, Blaha GR, Marx JL. Humphrey visual field findings in hydroxychloroquine toxicity. Eye. 2011 Dec;25(12):1535-45.



