PEER REVIEWED
Optic Nerve Compression due to Dolichoectasia
Payton Yerke Hansen, BS, Katelyn L. Seeley, BS, and Duane L. Tanner, OD
Abstract
Dolichoectasia is a vascular disease that is commonly associated with chronic hypertension. High blood pressure can cause deterioration of the tunica intima, which can lead to elongation, dilation and tortuosity of the blood vessels. Enlarged vessels can impinge on nerve fibers, disrupting action potential propagation. This condition is rare and has a poor prognosis when considering 5-year survival rate. Most cases are asymptomatic, which increases the patient’s risk. Accurate diagnosis and timely intervention are crucial for improved outcomes. We present a case of dolichoectasia affecting the optic nerve found during a routine follow-up appointment. This teaching case report emphasizes the importance of clinical decision-making and the use of diagnostic tests and imaging to effectively diagnose dolichoectasia.
Key Words: dolichoectasia, vascular disease, action potential, visual field defect
Background
Dolichoectasia is a progressive vascular disease characterized by the fusiform dilation and elongation of intracranial arteries.1,2,3,4 This condition is rare and has a poor prognosis when considering 5-year survival rate. Most cases are asymptomatic, increasing the patient’s risk. Accurate diagnosis and timely intervention are crucial for improved outcomes. Dolichoectasia is primarily associated with sustained systemic hypertension.3 Inherited connective tissue disorders, such as Ehlers-Danlos syndrome, can also lead to weakened vessel walls that contribute to the dilation and distension of the vessel.5 Chronic increased pressure within the arterial wall interferes with collagen and elastin integrity in the tunica intima.1 As the connective tissue structure degrades, the vessel begins to enlarge, compressing surrounding structures. The diagnosis of vertebrobasilar dolichoectasia requires the basilar artery, the most affected vessel, to have a minimum diameter of 4.5 mm and a vertical deviation of > 10mm from the expected course.1,2,3
Less than 10% of dolichoectasia cases present with clinical symptoms.1 In some cases, the elongated and distended intracranial arteries compress cranial nerves, which inhibits action potential propagation. This compression can cause variable neurologic deficits based on which nerves are compressed. Symptoms that have been associated with dolichoectasia include ischemia, central sleep apnea, cerebellar dysfunction, obstructive hydrocephalus, trigeminal neuralgia and motor defects1,2,3 Dolichoectasia increases the risk of ischemic or hemorrhagic stroke.2 The variable symptoms create difficulty with diagnosing and treating dolichoectasia. As a result, many cases are misdiagnosed.
While uncommon, if the dolichoectatic vessel compresses the optic nerve fibers, it disrupts the visual pathway and can lead to vision impairment.6 We present a case report of dolichoectasia involving the optic nerve in a 79-year-old White male. The case report is intended to serve as a teaching guide to assist optometry students, residents and practitioners in recognizing the clinical presentation of dolichoectasia and using a Humphrey 24-2 full-threshold visual field test to determine whether neurological disease is present.
Case Description
A 79-year-old White male presented at the Salt Lake City Veterans Administration Medical Center optometry clinic for a pigmentary glaucoma follow-up appointment on March 1, 2017 (initially diagnosed by a different provider in 2015). The patient also had a previous diagnosis of cataracts. Other significant medical history did not include a family history of glaucoma. The patient’s blood pressure measured 160/93 mmHg. He had been prescribed medication for systemic hypertension but had self-discontinued it 7 years prior. He also reported that he had white coat syndrome, so he monitored his blood pressure at home. His most recent blood pressure measurement was 132/78 mmHg 2 days before the appointment.
The patient’s medications were acetaminophen/oxycodone, 325/5 mg tablets twice a day as needed for pain; ketotifen ophthalmic drops twice a day for ocular allergies; latanoprost ophthalmic drops once a day for glaucoma; dextran artificial tear drops 4 times a day as needed for dry eyes; and sildenafil citrate for erectile dysfunction prior to sexual activity. Recent lipid profiles, glucose levels, complete blood count and hemoglobin A1c levels were within normal ranges.
The patient had previously been diagnosed with pigment dispersion glaucoma and associated transillumination defects. He had thinner than average corneas with corneal pachymetry measurements of 536 µm in the right eye and 529 µm in the left eye. Eyes with thinner corneas are known to have intraocular pressure (IOP) underestimated by 2-5 mmHg by applanation tonometry. Optical coherence tomography (OCT) showed significant thinning of the retinal nerve fiber layer in the superior-temporal and inferior-temporal sectors of both eyes. Asymmetrical cupping of the optic discs was observed. These tests were repeated as was a Humphrey 24-2 full-threshold visual field test. The results from the visual field test did not correlate with the OCT findings. Instead, there was a consistent yet progressing left incongruous homonymous visual field defect, indicating a possible neurological condition (Figure 1).
The patient also complained of headaches in the morning, but his IOP remained within normal range. He reported significantly clearer vision in the morning after awakening and that his vision worsened throughout the day. The patient was referred for an MRI of the brain and orbits with and without gadolinium contrast dye concentrating on the right parietal lobe and the orbits. The images showed tortuous and enlarged anterior and middle cerebral arteries that distended and bilaterally exerted a mass effect upon the optic chiasm and optic tracts (Figure 2). The anterior and middle cerebral arteries appeared to be dolichoectatic and resting on the floor of the third ventricle (Figure 3). This confirmed the diagnosis of dolichoectasia.
 Figure 1. Results of the Humphrey 24-2 full-threshold visual field test showing a left incongruous homonymous visual field defect. Click to enlarge |
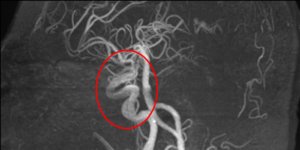 Figure 2. MRI of the dolichoectatic anterior cerebral arteries compressing the optic chiasm. Click to enlarge |
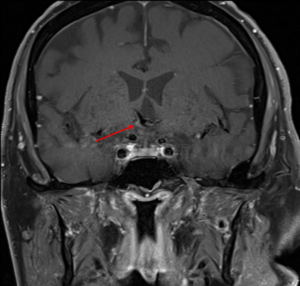 Figure 3. MRI of the dolichoectatic middle cerebral arteries visible under the floor of the third ventricle. Click to enlarge |
It was recommended that the patient resume taking medication to lower his blood pressure, but he refused. It remained uncertain whether he had glaucoma in addition to dolichoectasia. Due to this uncertainty, the patient was instructed to continue taking latanoprost and follow-up on his condition within 9 months. The patient underwent cataract extraction surgery. During that surgery, a micro-implant was placed into the trabecular meshwork of each eye to help improve aqueous outflow and control IOP. Once his eyes healed, the patient stopped taking latanoprost. After the diagnosis in 2017, his vision worsened, and debate continued among providers as to whether he had glaucoma in addition to dolichoectasia. In 2018, the patient suffered a non-fatal ischemic stroke.
Education Guidelines
Learning objectives
Students should be able to:
- describe why the clinical presentation of dolichoectasia can be so varied
- describe the causes of dolichoectasia
- recognize and describe how to know when visual field test findings indicate a likely neurological abnormality such as a mass or aneurysm
- accurately trace the visual pathway through the brain
- explain the relationship of the cerebral blood supply pathway to the visual pathway and identify areas where compression of visual fibers is most likely to occur
- acknowledge that a patient may have multiple conditions occurring at the same and create a list of differential diagnoses based on symptoms and examination findings
Key concepts
- dolichoectasia can cause vision impairment
- dolichoectasia can present clinical symptoms that are similar to those of other conditions
- patients can have multiple conditions occurring at the same time; therefore, a holistic approach is necessary for diagnosis
- dolichoectasia left untreated has a high morbidity and mortality rate
Discussion questions
- why does dolichoectasia often present with variable symptoms?
- why are most cases of dolichoectasia asymptomatic?
- why is dolichoectasia progressive?
- why does lateralization (field defects respect the vertical midline) on a visual field test indicate a possible neurological disorder?
- what is the vascular pathway of the internal carotid artery and the vertebral artery, and how do they relate anatomically to the cranial nerves?
- why was the patient’s vision affected in both eyes? How was vision affected? what vision symptoms may the patient have had?
- why did the patient’s vision improve after he had been lying down?
- why was the patient’s visual field defect crossing the vertical midline?
- how does dolichoectasia increase a patient’s risk for ischemic stroke?
Discussion
Literature review
Dolichoectasia is an uncommon but highly recognized vascular phenomenon that is seen more often in middle-age and elderly patients.3,7,8 It is also predominant in males.3,7 The disease preferentially affects the vertebral and basilar arteries, which was not observed in the case presented.3 We observed dolichoectasia in the right anterior and middle cerebral arteries.
Dolichoectasia has a poor prognosis with a 5-year survival rate. More than 90% of dolichoectasia cases are asymptomatic, and symptomatic cases vary in their clinical expressions.2,3 This places an increased burden on doctors to provide a correct diagnosis in a timely manner. Because blood flow is impeded, ischemia and a higher risk of ischemic and hemorrhagic strokes are commonly observed.2,5 It is not uncommon for intracranial bleeding to occur.9 The 3- to 5-year survival rate of those diagnosed with dolichoectasia is 60-70% with asymptomatic patients having a better prognosis.5,6,10,11
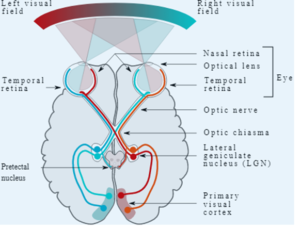
Figure 4. The primary visual pathway (solid lines). Source: Miquel Perello Nieto, CC BY-SA 4.0, via Wikimedia Commons. Click to enlarge
In some cases, the distended artery may compress cranial nerves, which leads to a variety of symptoms based on what nerve is hindered and at which position along its pathway the compression occurs (Figure 4). Common symptoms documented are hemifacial spasms and trigeminal neuralgia caused by the pulsatile compression of the facial nerve root and trigeminal nerve root.4 Other symptoms that may be observed are hearing loss, tinnitus and nystagmus caused by the compression of the vestibulocochlear nerve. Horner syndrome and diplopia may be caused by the compression of the oculomotor, abducens or trochlear nerves, and dysphagia when the medullary pyramids are constricted.4 In rare cases, vision loss and homonymous hemianopia are observed when there is a compression along the optic tracts.4 These conditions are uncommon because the cranial vasculature has less access to compress the nerves along the optic tracts. The potential for these events corresponds to the location, the severity of elongation, and dilation of the arterial wall.6,12
Dolichoectasia was originally regarded as an atherosclerotic disease, similar to aneurysms.1 Histological studies found that the basis of the pathology is chronic hypertension, which causes the degeneration of the internal elastic lamina as well as atrophy of vascular smooth muscle.3 This deterioration makes the disease highly progressive because as the vessel’s diameter increases, it creates a shift in pressure based on Poiseuille’s Law.13 In areas where the diameter is larger, the pressure pushing against the vessel walls increases.4 The differences in vessel diameter creates a bidirectional, turbulent blood flow that significantly increases the risk of thrombus formation and ischemia.5,14 Both symptomatic and asymptomatic patients need repeat imaging to monitor the progression of the disease and functional testing such as blink reflex, vision tests, brainstem auditory-evoked potentials and motor-evoked potentials.1 The most common management is controlling hypertension through medication and lifestyle changes.2 There are also surgical options for severe cases in which impaired cerebral spinal fluid circulation increases intracranial pressure. Most surgeries involve a ventriculoperitoneal shunt. If the vessel obstructs the foramen of Monro, a biventricular shunt is used instead.1 In cases similar to what we observed, some vision loss due to dolichoectasia can be regained through the surgical removal of the ectatic area of the vessel, decompressing the optic nerve by separating it from the vessel via interposition of muscle tissue, or de-roofing the optic canal and cutting the dural fold and sheath of the optic nerve.8 However, this last procedure is highly debated among practitioners.
Teaching methodology and assessment
This information could reasonably be covered in one or two 1-hour sessions. Students should spend approximately one-third of the allotted time working in a small group. Another one-third of the time should be devoted to self-study. A larger group wrap-up session should be completed during the last one-third of the time. The facilitator should lead the wrap-up session by choosing students at random to explain different portions of the case.
Participants should think critically about each discussion question using the information provided in the Background and Case Description. At the conclusion of the allotted time for review of the information provided, participants should submit their answers in an essay format. Their responses can be compared to the information below each question.
Why does dolichoectasia often have variable symptoms?
The clinical symptoms expressed depend on which cerebral nerves are compressed by dolichoectatic vessels and how it affects the antegrade blood flow in the system.10 Symptoms are based on the severity of the condition.
Why are most cases of dolichoectasia asymptomatic?
Symptoms arise due to the compression of nerves or the disruption of blood flow and are proportionate to the severity of the condition. Dolichoectatic vessels generally do not interfere with the cranial nerves, and they may not hinder the blood flow enough to cause ischemia or stroke.
Why was lateralization of the patient’s visual field incongruous?
The patient had multiple dolichoectatic vessels that interfered with his sight depending on the nerves compressed as well as where along the nerve pathway the compression was located. He also may have had glaucoma, which could have caused a portion of the visual field loss.
Why does lateralization of the field of vision indicate a neurological disorder?
Lateralized loss respecting the vertical midline in a patient’s field of vision is neurologically significant based on the structure of the optic pathway. Temporal vision fibers travel through the medial portion of the optic nerve to the optic chiasm, where they cross and continue to the occipital lobe. Nasal vision fibers travel through the lateral portion of the optic nerve to the optic chiasm. Lateralization in one or both eyes indicates that the optic pathway is disrupted. In our case, the patient experienced lateralization in both eyes. Because both eyes were affected, we knew there must be a chiasmal or post chiasmal location for the vascular compression. This was confirmed with an MRI scan.
What is the vascular pathway of the internal carotid artery and the vertebral artery, and how do they relate anatomically to the cranial nerves?
Blood supply to the brain comes from four main arteries, the two carotid and the two vertebral (Figure 5).
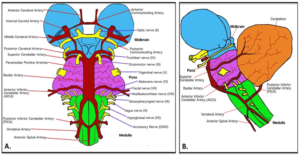
Figure 5. Brainstem vasculature and emerging cranial nerves. Source: Cuoco et al., Creative Commons Attribution 4.0 International License, via Edorium Journal of Neurology.15 Click to enlarge
The vertebral arteries travel up the lateral sides of the brainstem and then merge into one larger vessel, the basilar artery. The basilar artery continues up the anterior midline of the pons to the level of the midbrain where it connects into the circle of Willis. The arteries (inferior and superior cerebellar) and arterioles that branch off the vertebral and basilar arteries provide the blood supply to cranial nerves 3 through 12. When the basilar artery reaches the midbrain, it bifurcates into the posterior communicating arteries. These vessels connect with the internal carotid arteries. The carotids give rise to the middle and anterior cerebral arteries. The anterior communicating artery connects the two anterior cerebral arteries to complete the formation of the circle of Willis. The ophthalmic arteries are a bifurcation of both internal carotids. They supply the second cranial nerves. The anterior cerebral arteries supply the first cranial nerves.
Why was the patient’s vision affected in both eyes? How was vision affected? What vision symptoms may the patient have had?
Vision was affected in both eyes because of the architectural layout of the optic nerve fibers and their distribution throughout the visual pathway. At the optic chiasm, the nerve fibers from both eyes cross and then travel to the appropriate side of the brain and back to the visual cortex. When there is homonymous visual field loss in both eyes that respects the vertical midline, the lesion must be located at or posterior to the optic chiasm, affecting peripheral vision.
Why did the patient’s vision improve after he had been lying down?
The forces of gravity played a large part in the patient’s symptoms. In the supine position, gravity moved the distended blood vessel off the impinged visual nerve fibers. In the upright position, gravity moved the vessel back onto the affected visual nerve fibers causing the vision to be worse.
Why is dolichoectasia progressive?
As an artery increases in size, it forces the blood to travel from a large-diameter area to a small-diameter area. Based on Poiseuille’s Law, when liquid travels through a system with changing diameter, the velocity increases in the small-diameter area, and the pressure against the walls of the system increases in the area with a larger diameter.13 The increased shift in pressure against the dolichoectatic area of the vessel creates a larger force against the walls that can cause the intima to further deteriorate. This can lead to a progressive increase in diameter and elongation.
How does dolichoectasia increase a patient’s risk of ischemic or hemorrhagic stroke?
The dilated portions of arteries create a bidirectional flow, which causes a net reduction in blood flow leading to ischemia. The bidirectional current causes turbulence in the blood flow, which increases thrombus formation leading to stroke.10
Conclusion
This teaching case report is especially useful because it requires participants to consider multiple diseases and the anatomy and physiology of the visual system in order to correlate clinical findings to the patient’s actual condition. The clinician must use a variety of testing modalities to effectively accomplish this. The increased morbidity associated with undiagnosed dolichoectasia makes accurate identification and prompt treatment crucial. Multidisciplinary coordination and action are essential in reducing loss of function and extending the patient’s life.
References
- Kansal R, Mahore A, Dange N, Kukreja S. Dolichoectasia of vertebrobasilar arteries as a cause of hydrocephalus. J Neurosci Rural Pract. 2011 Jan;2(1):62-4. doi: 10.4103/0976-3147.80106.
- Lin YW, Chen CH, Lai ML. The dilemma of treating vertebrobasilar dolichoectasia. Clin Pract. 2012 Oct 17;2(4):e84. doi: 10.4081/cp.2012.e84.
- Yuh SJ, Alkherayf F, Lesiuk H. Dolichoectasia of the vertebral basilar and internal carotid arteries: a case report and literature review. Surg Neurol Int. 2013 Nov 29;4:153. doi: 10.4103/2152-7806.122397.
- Samim M, Goldstein A, Schindler J, Johnson MH. Multimodality imaging of vertebrobasilar dolichoectasia: clinical presentations and imaging spectrum. Radiographics. 2016 Jul-Aug;36(4):1129-46. doi: 10.1148/rg.2016150032.
- Ubogu EE, Zaidat OO. Vertebrobasilar dolichoectasia diagnosed by magnetic resonance angiography and risk of stroke and death: a cohort study. J Neurol Neurosurg Psychiatry. 2004 Jan;75(1):22-6.
- Blumenthal EZ, Gomori JM, Dotan S. Recurrent abducens nerve palsy caused by dolichoectasia of the cavernous internal carotid artery. Am J Ophthalmol. 1997 Aug;124(2):255-7. doi: 10.1016/s0002-9394(14)70799-8.
- Parera IC, Abruzzi M, Lehkuniec E, Schuster G, Muchnik S. [Dolichoectatic intracranial arteries. Advances in images and therapeutics]. Medicina. 1994;55(1):59-68.
- Huber A. Fusiform aneurysms (dolichoectasia) of the internal carotid artery as cause of optic nerve damage. Neuro-Ophthalmol. 2009;18(3):141-145.
- Passero SG, Calchetti B, Bartalini S. Intracranial bleeding in patients with vertebrobasilar dolichoectasia. Stroke. 2005 Jul;36(7):1421-5. doi: 10.1161/01.STR.0000172311.64662.9c.
- Milandre L, Bonnefoi B, Pestre P, Pellissier JF, Grisoli F, Khalil R. [Vertebrobasilar arterial dolichoectasia. Complications and prognosis]. Rev. Neurol (Paris). 1991;147(11):714-722.
- Wolters FJ, Rinkel GJ, Vergouwen MD. Clinical course and treatment of vertebrobasilar dolichoectasia: a systematic review of the literature. Neurol Res. 2013 Mar;35(2):131-7. doi: 10.1179/1743132812Y.0000000149.
- Passero SG, Rossi S. Natural history of vertebrobasilar dolichoectasia. Neurology. 2008 Jan 1;70(1):66-72. doi: 10.1212/01.wnl.0000286947.89193.f3.
- Sadahiro H, Ishihara H, Goto H, et al. Repeated cerebral ischemia caused by extracranial carotid artery dolichoectasia. J Neuroimaging. 2014 Jan-Feb;24(1):83-7. doi: 10.1111/j.1552-6569.2011.00656.x.
- Lou M, Caplan LR. Vertebrobasilar dilatative arteriopathy (dolichoectasia). Ann N Y Acad Sci. 2010 Jan;1184:121-33. doi: 10.1111/j.1749-6632.2009.05114.x.
- Cuoco JA, Hitscherich K, Hoehmann CL. Brainstem vascular syndromes: a practical guide for medical students. Edorium J Neurol 2016;3:4-16. doi:10.5348/N06-2016-8-RA-2.



