Optometry Students’ Knowledge-Based Performance within Interprofessional Education Courses
Jasmine W. Yumori, OD, FAAO, David N. Dickter, PhD, Kierstyn Napier-Dovorany, OD, FAAO, Valerie Q. Wren, OD, FAAO, John H. Tegzes, MA, VMD, Dipl. ABVT, Sorrel Stielstra, PhD
Abstract
Background: Collaborative team-based health care has been shown to improve healthcare safety and quality. An approach to building a collaborative team-based healthcare environment includes increasing opportunities for interprofessional training. Our objective is to assess optometry students’ knowledge-based performance in an interprofessional education (IPE) course.
Methods: We performed a retrospective observational study with students enrolled in Phase I courses of the IPE program at Western University of Health Sciences. Student performance was assessed using a multiple-choice question (MCQ) examination on concepts related to IPE. We compared pre-course and post-course scores from the 2013-2014 academic year for optometry students and all others enrolled in the courses.
Results: 85 first-year optometry students and 726 students from other graduate health professions programs completed both the pre-course and post-course MCQ examination. The mean pre-course score was 35±9 (17-53) percent for optometry students and 38±10 (3-83) percent for all others (statistically significant difference, t(809)=2.1, p<.05). The mean post-course score was 71±15 (33-90) percent among optometry students; the mean post-course score was 70±14 (3-90) percent among all others combined (not a statistically significant difference). Pre-post course scores increased significantly for both optometry students (paired-sample t(84)=20.7, p<.001) and all other students (paired-sample t(725)=48.0, p<.001).
Conclusion: Although it has been recognized that teamwork and collaboration between healthcare providers is important to improve healthcare delivery, IPE experiences, particularly those involving optometry students, are limited. This study shows that optometry students benefit from and can comparably perform in knowledge-based acquisition of concepts within IPE courses alongside students from other health professions. There is a need for more interprofessional training and tools to better assess student performance.
Key Words: interprofessional education, multiple-choice question examination, optometry students
Background
Introduction
The World Health Organization has emphasized the importance of preparing the healthcare workforce for teamwork and collaboration between healthcare providers and between providers and patients.1 According to the Institute of Medicine (IOM), there are as many as 98,000 deaths annually due to medical errors in hospitals,2 including preventable errors caused by failure of communication.3 The IOM has emphasized the importance of interdisciplinary training for improving healthcare delivery.4 In the United States, a number of factors have set the stage for the IOM’s calls for interprofessional, community-based programs and health professions curricula.5 These include an aging population and a growing number of patients with chronic diseases and conditions1as well as a shift in focus to community-based health and medical homes for disease prevention and health promotion associated with the Affordable Care Act of 2010.5 Interprofessional teams can reduce medical errors, enhance quality of care and patient satisfaction, lower cost, and decrease the length of stay in patient care facilities.6, 7 In order to fulfill these expectations, interprofessional experiences are needed to provide students with the skills and opportunities to communicate, negotiate, employ shared leadership and decision-making, and engage in conflict resolution when needed.7
Interprofessional education and optometry
Interprofessional education (IPE) takes place when “two or more professions learn with, from, and about each other to improve collaboration and the quality of care.”8 Optometry is essential to the healthcare team for its unique scope of practice, relationship with patients and ability to diagnose and treat ocular and visual disorders as well as detect systemic diseases that affect the eye.9 Opportunities for collaborative education and practice within optometry have grown, with 19 of 21 members of the Association of Schools and Colleges of Optometry (ASCO) reporting participation in IPE activities and nine reporting IPE as a program requirement.10 All optometry programs may take advantage of fourth-year clinical rotations at multidisciplinary settings such as Veterans Affairs medical facilities offering interactions with medicine, nursing, pharmacy, dentistry and other professions.11
Interprofessional education figures prominently in the ASCO report on the expectations for optometry curricula.12 As quoted from ASCO’s “Attributes of Graduates of the Schools and Colleges of Optometry (2011),” graduates are expected to:
● have the ability to appropriately use all resources, including ancillary personnel, intraprofessional and interprofessional collaboration, co-management and referral, in ensuring the best quality patient care
● manage their practices in a manner that is appropriate within the healthcare delivery system and that promotes patient access to eye and vision care
● have the ability to recognize personal limitations regarding optimal patient care and to work with the broader healthcare community in providing the best care possible
● have a commitment to work as an integral member of the larger interprofessional healthcare team to improve patient care outcomes
● have the ability to recognize and initiate the coordination of patient care requiring advanced medical, systemic, interprofessional or specialty care
● have the ability to work in cooperation with those who receive care, those who provide care, and others who contribute to or support the delivery of prevention and health services.
The above expectations are in alignment with the Core Competencies outlined by the Interprofessional Education Collaborative (IPEC), a coalition of health professions education organizations and associations, of which ASCO was the first supporting organization.”11 The Core Competencies for Interprofessional Collaborative Practice13 from the Collaborative are seen in Table 1. These competencies apply to the practice of all health professions and shed light on the requirements for IPE that can help guide optometric education.
Interprofessional education at Western University of Health Sciences
Western University of Health Sciences is a fully accredited non-profit private graduate school focused on the health professions that offers 22 academic programs in nine health sciences colleges: optometry, dental medicine, nursing, osteopathic medicine, pharmacy, physician assistant studies, physical therapy, podiatric medicine and veterinary medicine.14
The mission of the IPE program at Western University of Health Sciences is to “produce humanistic healthcare professionals who provide and promote collaborative patient-centered care and coordinated healthcare management.”15 Graduates are expected to demonstrate an understanding of the roles and responsibilities of other health professionals.16 They must also demonstrate a realization that each healthcare profession possesses unique skills and perspectives that can improve the quality and safety of health care. These expectations are highlighted in the IPE program competencies, which are outlined in Table 2. These overlap with and augment the IPEC competencies listed in Table 1.
All students across the nine health sciences colleges are required to participate in the IPE program; 947 students participated in the Phase I IPE courses during the 2013-2014 academic year. The IPE curriculum also includes Phases II and III. To date, every Western University of Health Sciences College of Optometry student has completed all three phases with students from other health professions.
Phase I
Currently delivered as a required two-semester course, Phase I launched in January 2010 and involves all first-year students in the nine colleges at Western University of Health Sciences. While Phase I introduces students to all of the IPE program competencies seen in Table 2, the main foci are to introduce students to other professions and their respective scopes of practice and to help students understand the concepts of team-based, collaborative communication and care. Knowledge and understanding of the healthcare team, patient-centered care, teamwork, and interspecies similarities, differences and interactions are also explored. The IPE program competencies are shared and practiced while the students interactively and collaboratively review a case scenario featuring general health issues of significant medical relevance. The health issues for the 2013-2014 academic year that all of the students covered were:
● diabetes / obesity
● infectious disease / one health
● neurodegenerative disease
● neurodevelopment / autism
● cancer / end-of-life care

Photograph 1. An interprofessional small group meeting from IPE Phase I.
Each case scenario is covered over three 90-minute group meetings held one week apart (Table 3).
During the first week, students participate in an intraprofessional meeting on the health issue, focusing on aspects most relevant to their profession. In the second and third weeks, the students meet in pre-assigned interprofessional groups of approximately 10 students plus a trained facilitator (Photograph 1) to work through each case scenario, focusing on patient safety and quality of care issues. An excerpt from a previous Phase I case is found in the Appendix.
The interprofessional small group meetings are designed for students to interact and thus develop and practice interprofessional collaboration skills and behaviors. To ensure that facilitators are able to appropriately provide feedback and guidance to students, facilitator training is mandatory for involvement in Phase I.
College of Optometry student involvement
Optometry students participate in Phase I in the same way that all other students do. They participate in all aspects of the program and are equal members of the team. The first of the three sessions is the intraprofessional session, which is delivered by a College of Optometry faculty member who is also a practicing optometrist. She provides profession-specific background information for each case, focusing particular attention on the visual and ocular effects of the disease process. For example, in the obesity and diabetes case, information and resources regarding diabetic eye disease is shared. In the second and third sessions, optometry students participate as equal members of the small group interprofessional teams along with students from the other programs.
College of Optometry faculty involvement
Complementing the extensive student involvement in the IPE curriculum, all of the faculty members and administrators at the College of Optometry have been trained in IPE facilitation to support Phase I. Out of the entire College of Optometry faculty, 94% of faculty members have participated in at least one phase of the IPE curriculum. Development of facilitation skills is continuously supported, as exemplified by session briefings before each case and written facilitator information provided prior to each case session. In addition to facilitating for Phase I, College of Optometry faculty members also serve as case authors for Phase II, help design and evaluate case simulation sessions from Phase III (Photograph 2), and provide guidance for the development beyond Phase III.
Three optometry faculty members have additional responsibilities within the IPE curriculum as liaisons to the IPE department for the college. These faculty members act as representatives of the college and provide input on curriculum development, implementation and assessment. These faculty members lead the intraprofessional sessions for optometry students during Phases I and II and provide support for optometry students during Phase III. They also actively participate in the monthly IPE design team meetings with liaisons from the other colleges and IPE department faculty, and act as contacts for optometry students and faculty who are involved in each phase of the program. Another optometry faculty member, Dr. Jasmine Yumori, has a joint appointment between the College of Optometry and the IPE department. Within the IPE department Dr. Yumori serves as one of the Co-Directors of IPE Phases I and II at the university level.
In addition to providing an overview of IPE at Western University of Health Sciences and its relevance to optometry, we also investigated whether optometry students participating in Phase I of the IPE program during the 2013-2014 academic year acquired knowledge based on IPE competencies compared with students from other health professions.
Methods
In the IPE Phase 1 courses, students were evaluated in part by their performance on a multiple-choice question (MCQ) examination given at the start of the course and again at the end of the course (identical items). Taking both the pre- and post-course examinations was not mandatory; however, 86% (811 of 947) completed both.
A MCQ examination based on the Western University of Health Sciences IPE program competencies was constructed. The examination consisted of 30 multiple-choice questions split between the five competencies: Scope of Practice (primary focus of examination; 17 items), Communication (3 items), Collaboration (4 items), Team Skills (4 items) and One Health (2 items). The following MCQ types were used:
● A-type: Students are provided with a clinical scenario, lead-in questions and a list of possible responses with one correct answer.
● X-type: Students are provided with a short introductory stem and one or more correct answers.
Examination design was led by Dr. John Tegzes, Director of IPE at Western University of Health Sciences, and Dr. David Dickter, IPE Research Director at Western University of Health Sciences, with faculty members from all nine of the health professions colleges providing input and feedback on the examination.
Students individually completed the MCQ examination at the beginning of the course. Feedback was not provided to students after the pre-course examination since students also completed the same examination at the end of the course. Once students completed the post-course examination they were invited to individually discuss and receive feedback on the content.
Data were analyzed using IBM SPSS version 12.0 to conduct descriptive statistics (mean, standard deviation, range) and analytical statistics (paired and two-sample t-tests).
Results
The MCQ examination was administered to all students enrolled in the Phase I courses of the IPE program during the 2013-2014 academic year at Western University of Health Sciences. A total of 811 students completed all items on both the pre-course and post-course MCQ examinations (85 from the College of Optometry and 726 from the other programs combined). Note that it was possible to pass the course without completing the examinations (e.g., students could remediate through other assignments).
The pre-course mean performance on the MCQ exam for optometry students was 35±9 (17-53) percent; the pre-course mean performance for all other students combined was 38±10 (3-83) percent. This difference in overall MCQ scores was statistically significant (t(809)=2.1, p<.05). Table 4 displays the results by competency. Results were similar across the competencies, with the students answering approximately 30-40% of the questions correctly.
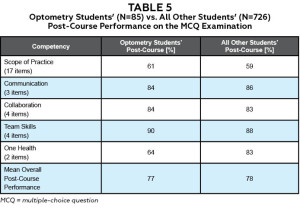
The post-course mean performance on the MCQ exam for optometry students was not statistically different from those of all other students combined. On average, optometry students answered 71±15 (33-90) percent correctly; the other students answered 70±14 (3-90) percent correctly. Total MCQ exam pre-post course scores increased significantly for both optometry students (from 35% to 71%; paired-sample t(84)=20.7, p<.001) and all other students combined (from 38% to 70%; paired-sample t(725)=48.0, p<.001). Students demonstrated the strongest post-course performance on questions related to Team Skills and Communication (Table 5).
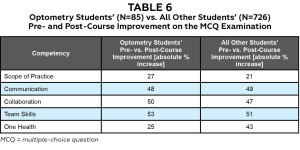
As shown in Table 6, improvement was evident across all five competency domains for optometry and all students. Due to the relatively small number of items measuring each competency, we limited our analysis to trends observed rather than statistical difference tests. Team Skills questions were associated with the highest pre- vs. post-course improvement trends. Moderate to strong improvement trends (25 to 53 absolute percentage point increases) were seen for all competencies for optometry students.
Discussion
The mean pre-course MCQ examination scores for all students suggest that students from all graduate health professions can benefit from participation in IPE courses. The somewhat lower (35% vs. 38%) baseline (pre-course) differences in knowledge between optometry and other students might stem from differences in pre-course exposures to other health professions for students interested in optometry, which is traditionally more outpatient-focused. Interestingly, the performance of optometry students on the post-course MCQ examination was comparable to the performance seen for all students.
Based on the pre- vs. post-course MCQ examination scores, optometry students benefit from and perform comparably to students from other health professions and should be included in IPE courses. As student scores increased the most on Team Skills and Communication competencies, it may be that these are among the most trainable for IPE students at the introductory graduate level. More investigation is needed to confirm these findings and determine possible implications.
One of the limitations of the pre- and post-course MCQ examinations was lack of a control group. It would be interesting to examine students’ performance on the MCQ examinations taken at the same time interval and environment but without exposure to our IPE courses to determine whether the improvements may be attributable to the effectiveness of the program vs. other causes such as natural maturation and/or improved readiness during the post-test due to knowledge absorption from the pre-test. Further development of the MCQ examination is also needed, as is the collection of reliability and validity data.
Conclusion
Education on team-based health care is important for improving patient safety and addressing quality of care issues. The profession of optometry plays an important role on the healthcare team. Optometry students benefit from and can comparably perform in IPE courses alongside students from other health professions.
The development of additional opportunities for students to further develop an understanding of and application of IPE competencies is crucial. Similarly, the creation of additional tools to better assess student performance associated with IPE competencies is also needed. Developers of optometry and IPE curricula should collect information on skills acquisition, for example, based on simulated patient encounters and clinical performance ratings from multiple sources (e.g., self, peer and clinical supervisors). Further research is needed to understand how knowledge acquisition translates into the ability to demonstrate the skills and behaviors needed to function successfully in interprofessional team settings.
Acknowledgements
We wish to thank the following people for their support and review of content in this paper: Sheree Aston, OD, MA, PhD, Vice Provost, Chair of the IPE Initiative, and Co-founder of the IPE program; Elizabeth Hoppe, OD, DrPH, Founding Dean of the College of Optometry and strong proponent of the IPE program; and Pat Callard, MSN, RN, CNE, CNL, Assistant Professor at the College of Graduate Nursing and Co-Course Director of IPE Phases I and II.
References
1. World Health Organization. The World Health Report 2006: Working Together for Health. Geneva, Switzerland: 2006.
2. Institute of Medicine. To Err is Human: Building a Safer Health System. November 1999. [cited 2014 May 29]. Available from: https://www.iom.edu/~/media/Files/Report%20Files/1999/To-Err-is-Human/To%20Err%20is%20Human%201999%20%20report%20brief.pdf.
3. Leape LL, Lawthers AG, Brennan TA, Johnson WG. Preventing medical injury. QRB Qual Rev Bull. 1993;19(5):144-9.
4. Institute of Medicine. Crossing the Quality Chasm: A New Health System for the 21st Century. March 2001. [cited 2014 May 29]. Available from: https://www.iom.edu/~/media/Files/Report%20Files/2001/Crossing-the-Quality-Chasm/Quality%20Chasm%202001%20%20report%20brief.pdf.
5. Institute of Medicine. Scaling Up Best Practices in Community-Based Health Professional Education: A Workshop. May 2014. [cited 2014 August 1]. Available from: https://www.iom.edu/Activities/Global/InnovationHealthProfEducation/2014-MAY-01.aspx.
6. Reeves S, Goldman J, Burton A, Sawatzky-Girling B. Synthesis of systematic review evidence of interprofessional education. J Allied Health. 2010 Fall;39 Suppl 1:198-203.
7. Packard K, Chehal H, Maio A, Doll J, Furze J, Huggett K, et al. Interprofessional team reasoning framework as a tool for case study analysis with health professions students: a randomized study. Journal of Research in Interprofessional Practice and Education. 2012;2(3):250-263.
8. Centre for The Advancement of Interprofessional Education. Defining IPE 2002. Available from: https://caipe.org.uk/about-us/defining-ipe/.
9. American Optometric Association. What is a Doctor of Optometry? 2012 [cited 2014 June 2]. Available from: https://www.aoa.org/about-the-aoa/what-is-a-doctor-of-optometry?sso=y.
10. Baker JL, Vitek MA. Interprofessional education and collaborative patient Care at U.S. schools and colleges of optometry: a special report. Optometric Education. 2015;40(2):72-6.
11. Association of Schools and Colleges of Optometry. Interprofessional Education 2013 [cited 2014 May 30]. Available from: https://www.opted.org/partnerships-advocacy/interprofessional-education/.
12. Association of Schools and Colleges of Optometry. Attributes of Students Graduating from Schools and Colleges of Optometry 2011 [cited 2014 May 30]. Available from: https://www.opted.org/files/2011_AttributesReport.pdf.
13. Interprofessional Education Collaborative Expert Panel. Core Competencies for Interprofessional Collaborative Practice: Report of an Expert Panel. 2011.
14. Western University of Health Sciences. About Western University of Health Sciences 2014 [cited 2014 August 28]. Available from: https://www.westernu.edu/university/university-about/.
15. Western University of Health Sciences WP. IPE Initiative Mission Statement 2014 [cited 2014 August 1]. Available from: https://www.westernu.edu/interprofessional/interprofessional-about/interprofessional-mission/.
16. Aston S, Rheault W, Arenson CF, Tappert S, Stoeker J, Orzoff J, Galitski H, Mackintosh S. Interprofessional education: a review and analysis of programs from three academic health centers. S Acad Med. 2012;87(7):1-7.