Pilot Assessment of Teaching Anterior Segment Evaluation to Develop Interprofessional Education Programs
Andrew McLeod OD, MS, FAAO, Sara Bush, OD
Abstract
Background: Interprofessional education (IPE) is proposed to lead to better learner outcomes, a collaborative practice environment and improved patient outcomes. This investigation aimed to increase knowledge and experience levels with anterior segment evaluation techniques. Methods: The School of Optometry at MCPHS University conducted a workshop and administered surveys to Physician Assistant Studies students. Results: Survey results (n=88) showed a significant increase (p<0.0001) in self-reported knowledge and experience from before to after the workshop and favorable views of IPE. Conclusions: The workshop was an effective format to increase knowledge and experience and provided information for planning future IPE programs.
Key Words: interprofessional education, anterior segment, optometric education, physician assistant education, optometry
Background
In medically based practice, frustration and confusion can occur during communication between specialty services and more general or diverse services. In most of these instances, the generalist is trying to receive a consultation in his or her department or trying to refer a patient to a specialized service. It can be difficult for the specialist to triage the patient if the referring providers are unable to supply the information requested or simply unsure what testing is necessary. In the case of optometry and ophthalmology, this often occurs when we request specialized testing such as visual acuity, intraocular pressure measurement, slit-lamp examination or retinal evaluation from referring doctors in order to better triage the patient.
Many health professions, including optometry, have traditionally educated their students in isolation. The assumption was the professions would somehow all learn to interact with each other upon entering the workplace. The four newest optometric programs are within multidisciplinary health science universities (Western University of Health Sciences in Pomona, Calif.; Midwestern University in Glendale, Ariz.; University of the Incarnate Word in San Antonio, Texas; and MCPHS University in Worcester, Mass.). Other programs, such as Pennsylvania College of Optometry and Southern California College of Optometry, have expanded to form multidisciplinary institutions (Salus University in Elkins Park, Pa., and Marshall B. Ketchum University in Fullerton, Calif., respectively). While the vast majority of these programs are still conducted in isolation, the multidisciplinary setup allows possible bridges between the programs to be formed.
Within health care, the variety, role and privileges of each health professional are continuing to expand and overlap. Some professionals prefer to keep skill sets within their specialty and to be taught only by individuals from their profession. The current trend, however, is toward an interprofessional approach to education, which is defined slightly differently by organizations. The Centre for the Advancement of Interprofessional Education states that interprofessional education (IPE) occurs when two or more professions learn with, from and about each other to improve collaboration and the quality of care.1 The World Health Organization defines IPE as when students from two or more professions learn about, from and with each other to enable effective collaboration and improve health outcomes.2 Although these definitions can be interpreted in different ways, the end goal of IPE should allow for discussion on how the professions will interact. IPE is not simply sharing a joint lecture or being taught by a different healthcare professional without discussion on how it will impact future collaborative care. IPE is an active learning process with other interprofessional students, not simply a passive learning process among other interprofessional students. In 2008, the Interprofessional Education Collaborative developed Core Competencies for Interprofessional Collaborative Practice.3 This Collaborative had representation from major organizations in nursing, osteopathic medicine, pharmacy, dental education, medical colleges and public health. Although it did not have optometry representation, it is a valuable framework for developing programs. In 2005, Oandasan and Reeves also reviewed the literature and provided a valid framework for the success of future IPE programs.4,5
The main initiative behind converting to an IPE environment is that it will lead to better learner outcomes that, in turn, will lead to a collaborative practice environment and better patient outcomes.2 The hope is to provide safer, timelier, more cost effective and more collaborative patient-centered care. A 2008 Cochrane Collaboration review of the effectiveness of IPE on health outcomes reviewed and assessed a series of IPE intervention studies published between 1999 and 2006. Of the 1,801 abstracts found, the review found only six intervention studies that met the inclusion criteria. Although four resulted in positive outcomes, the general conclusion was that it was not possible to draw generalizable inferences about the key elements of IPE and its effectiveness.6
Although IPE has been under discussion for years, there have been very few articles that deal with the profession of optometry. In April 2012, Michigan College of Optometry reviewed its Interprofessional Wellness Clinic, which also focuses on diabetes. The program integrates nursing, pharmacy and optometry services and has been in existence since 2004.7 In July 2012, a review of the Western University design and outcomes was published. It describes the university’s three-phase approach to IPE through didactic, online simulations and clinical care in the Western Diabetes Institute.8 Diabetes is a logical entry point for IPE as it is a relatively common condition and the patients typically visit multiple providers for care of the same condition. In August 2014, University of Alabama at Birmingham Geriatric Education Center created an Interprofessional Clinical Experience in nursing homes that included optometry students. The investigation found health professions trainees’ attitudes toward IPE and team care were positive after participating in the program.9
The American Optometric Association defines an optometrist as an independent primary healthcare professional for the eye. Since the expansion of optometry’s scope of practice to a more medical model, more optometrists are practicing in interprofessional settings such as nursing homes, community health centers and hospital-based practices. Therefore, optometry graduates could be more well-served and prepared for these practice settings through curricula that include IPE.
MCPHS University offers multiple professional healthcare programs, but the majority of each program is taught in isolation. The pilot workshop design was an attempt to initiate the move toward IPE between the School of Optometry and the School of Physician Assistant Studies. The objective of this pilot was not to create expertise in the area of ocular examination for the physician assistant (PA) students, but to introduce basic concepts and techniques. While interprofessional collaboration was introduced, a future workshop was proposed with students from both schools focusing on improved communication and more efficient and appropriate referrals to optometry. It is very important for the PA students to know how to complete an ocular assessment and determine what is normal vs. abnormal in order to foster such referrals. Therefore, it is appropriate for the person educating these students to be an optometrist, the professional to whom they would be making a referral. Additionally, the PA faculty may have also had limited exposure to these techniques in school, leading to some level of discomfort in teaching the skills. Again, it would make sense to recruit faculty members from other programs who are experts in the area and are more comfortable and experienced teaching the techniques.
The logical first step to facilitating future collaborations between the PA and optometry students would be to introduce the techniques to both groups to make sure that the terminology used is familiar to both groups. This can be a difficult task when both groups need to know the material in different depths. For the optometry program, there are multiple lectures that cover all aspects of anterior segment evaluation because it will be done on almost every patient. For the PA students, while this is one of the many skills they may cover in clinical rotations, they will likely not cover it in as much depth or have multiple opportunities to perform it. Therefore, technical use of the slit lamp and completion of a general assessment of the eye was one goal of the program. Common techniques were selected that would aid in assessment and give pertinent information for a referral. Slit-lamp examination (Topcon Medical Systems Inc., Oakland N.J.) including sodium fluorescein staining and lid eversion, intraocular pressure by Tonopen AVIA (Reichert Technologies, Depew, N.Y.) and ocular irrigation were selected.
While this workshop did not have students from both programs participating, the faculty from the optometry program taught a condensed workshop-style curriculum reflective of the courses from the optometric curriculum on the same topics. This workshop provided the foundation to start further discussions or workshops on referral communication, other pertinent techniques or diagnosis/treatment/management.
Methods
Developing the workshop was divided into three main stages: pre-workshop organization, the workshop itself and post-workshop feedback analysis. Before the workshop began there was significant correspondence between the physician assistant and optometry programs in the form of meetings and e-mail. The only disclosure received was that the participants were introduced to the eye and ocular examination, but could have had varied experience on their clinical rotations. This possible variability in the target audience made planning the workshop slightly more difficult and forced the instructors to start at a basic level of ocular anatomy and simple slit-lamp mechanics.
As stated, the techniques focused on were ocular anatomy, slit-lamp examination, sodium fluorescein staining, lid eversion, drop instillation, intraocular pressure measurement and ocular irrigation. Participants were also given alternative ways to assess ocular health without specialty equipment. For example, a demonstration on how to use the 20D lens, with or without cobalt blue filter, in the direct ophthalmoscope in lieu of a slit lamp was included. This cohort of tests was chosen to maximize the use of the specialty equipment in the lab and focus on techniques that would be more challenging to teach in a non-optometry lab setting. These are also the most likely needed tests in an emergency or primary care type setting along with visual acuity. The introduction lecture was created to outline basic anatomy, slit-lamp description and technique, lid eversion and common normal and abnormal findings. The next segment included drop instillation, sodium fluorescein evaluation and ocular irrigation. After each lecture section, there was designated, immediate practice time for those techniques with supervision from optometry faculty. All materials, diagrams and videos were uploaded to the learning management system for future reference. Because the workshop was held in a short time frame of approximately two-hour sessions, more optometry faculty were recruited to keep the ratio 1 faculty:2 lanes, with each lane holding two to three PA students. Extra handheld equipment was borrowed to ensure time was not wasted waiting for equipment.
In order to obtain feedback and assess the effectiveness of the workshop, an exit survey was developed in which the students rated their didactic knowledge and actual experience with each of the six topics (ocular anatomy, slit-lamp examination, tonometry, fluorescein staining, drop instillation and ocular irrigation). A 0-5 scale (0=Never heard of the topic, 3=Moderate, 5= Thoroughly understood the topic) was used to allow the participants to rate their assessments. Five additional statements were presented, and the students rated their agreement with those based on the scale (5-Strongly Agree, 4-Somewhat Agree, 3-Neutral, 2-Somewhat Disagree and 1-Disagree). The statements were:
1) I feel interprofessional education (between different disciplines) enhances my educational experience
2) I feel there is adequate interprofessional education at MCPHS University
3) I feel the topics covered today are relevant to my postgraduate career
4) I feel the format of the workshop was appropriate for covering the topics
5) I feel it was more beneficial to my education to learn these techniques from optometrists rather than an educator in my discipline.
An open section for comments and suggestions was also added to obtain any other information the participants were willing to share. The project was approved (IRB011014M) by the MCPHS Institutional Review Board.
The workshop was part of the Physician Assistant Studies Professional Seminar Series. This is a periodic day for final-year students (n=116) to return from clinical rotations to campus to learn and refresh their knowledge of different skills. This particular seminar included four workshops: Optometry, Wound Care, Oral Health, and Spirometry. The seminar day included four sessions of each workshop each lasting two hours, thus each workshop was conducted four times during the day. The MCPHS University optometry facility includes two separate eight-lane pre-clinic spaces. Having one student act as the examiner and one as the patient, accommodations were available for up to 32 students per session. Three optometry faculty circulated each room along with any available PA faculty. Because of the separate rooms, the lecture was conducted in one pre-clinic area and web conferenced live to the other pre-clinic area via Blackboard Collaborate (Blackboard Inc., Washington D.C.) to ensure both labs had a more uniform experience. In addition to the main projection screens, the lecture was broadcast to each individual lane in both rooms. At the end of the workshop the surveys were distributed with the caveat that their participation in filling them out was optional.
Results
Prior to the workshop, 116 students were scheduled to attend the workshop and 108 students actually attended a workshop session. Of these, 99 filled out the optional survey, but only 88 had complete surveys (n=88). The 11 incomplete surveys were missing responses to the five statements regarding opinions on IPE, and were likely missed because they were on the back of the survey sheet. All surveys were completed at the end of the workshop, meaning the before and after responses were entered at the same time.
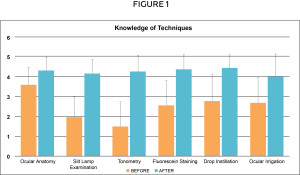
Click image to enlarge
Survey results (n=88) pertaining to self-reported knowledge level with techniques before and after the workshop. The 0-5 scale used was 0=Never heard of the topic, 3=Moderate, 5=Thoroughly understood the topic. The increase in knowledge level with each technique is statistically significant in each category (p<0.0001).
Knowledge and experience were compared from before to after the workshop using paired t-test and Bonferroni correction (k=12). Figure 1 outlines the responses for the self-rated amount of knowledge with ocular anatomy and the five techniques before and after the workshop. Statistical analysis shows a significant difference in responses from before to after (all ps<0.0001 after Bonferroni correction). Figure 2 outlines the responses for the self-rated amount of experience with each technique before and after the workshop. Statistical analysis again shows a significant difference from before to after (all ps<0.0001 after Bonferroni correction). Both knowledge and experience levels correlated in that ocular anatomy was the most familiar, while tonometry was the least familiar. After the workshop, the average response for knowledge and experience was raised to between 4 and 5, just below a thorough understanding level. The only exception was experience with ocular irrigation, which is most likely due to time limitations at the end of the session preventing many students from being able to attempt that technique.
Figure 3 outlines the average responses to questions pertaining to IPE and the workshop format. Responses indicate a positive attitude toward IPE and the level of IPE at MCPHS University. The students also had a positive response to the hands-on workshop format to enhance their education and appreciated being taught by instructors from other professions.
The majority of the responses in the comment section were to express their gratitude for the School of Optometry for conducting the workshop and satisfaction with the format. Several suggestions were made to have the optometrists conduct the introduction lecture(s) in the students’ didactic year, learn the techniques prior to rotations, repeat the workshops annually, and expand the topics to include fundoscopy or foreign body removal.
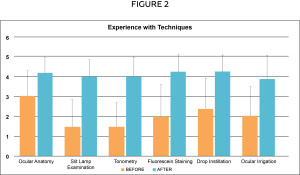
Click image to enlarge
Survey results (n=88) pertaining to self-reported experience level with techniques before and after the workshop. The 0-5 scale used was 0=Never heard of the topic, 3=Moderate, 5=Thoroughly understood the topic. The increase in experience level with each technique is statistically significant in each category (p<0.0001).
Discussion
Data analysis indicated that of the topics covered, the PA students had the most optometrically relevant knowledge and experience in ocular anatomy prior to the workshop. One would anticipate this because anatomy is part of the curriculum of all programs at MCPHS University. In addition, the terms discussed were basic anterior segment anatomy, of which many terms are used in lay conversation. Drop instillation, ocular irrigation and fluorescein staining were the next most familiar. This could be a result of teaching within their program or use in everyday life. These techniques can be taught without the use of highly specialized equipment and are probably done in a variety of clinical settings (primary care office, emergency room or hospital). The least amount of knowledge and experience was reported with slit lamp and tonometry. These procedures are most often utilized by eyecare professionals and require specialized equipment, so the limited exposure is understandable.
The reported amount of knowledge and experience increased in all categories after the workshop. The post-workshop experience and knowledge in ocular irrigation had a slightly lower result compared with the other tests. This can be attributed to the fact that in one session the lecture portion covering this material was not completed due to time constraints. In several sessions some of the students reported that they ran out of practice time for this technique. The higher results also indicate that the lecture coverage of the materials provided a thorough understanding of the topics. The hands-on workshop gave participants enough experience to feel more comfortable with performing techniques. This anecdotal response does not ensure proper or safe technique. A traditional proficiency-style practical exam or requirement to perform the technique a given amount of times under supervision may be better options.
The responses for statements 1 (I feel interprofessional education [between different disciplines] enhances my educational experience) and 5 (I feel it was more beneficial to my education to learn these techniques from optometrists rather than an educator in my discipline) indicate that the students like the idea of IPE and prefer being taught by professionals from the specialty area. This is probably true of professions, like physician assistant, which are cross-trained in many areas of health care. Statement 2 (I feel there is adequate interprofessional education at MCPHS University) had a wide variety of responses and the lowest overall average. A lower average response was anticipated, but perhaps some feel the amount of IPE is adequate while others wish there was more IPE. One of the survey responses indicated that PA students receive pharmacy education from pharmacists and pathology from pathologists, so why not eye care from optometrists. In addition, the complete, full-day seminar also included education from nursing, dental hygiene, physician assistant and optometry. The question 3 (I feel the topics covered today are relevant to my postgraduate career) results indicate the students feel the topics are relevant to their profession and would be useful after graduation. The average response to question 4 (I feel the format of the workshop was appropriate for covering the topics) indicates that the lecture/hands-on workshop format is successful for the students’ learning styles.

Click image to enlarge
Average responses to the statements surveyed regarding interprofessional education and workshop format (n=88).
This initial pilot design and investigation has limitations, but obtained a starting point for future collaborations. Due to the two-hour time constraint of the workshop, the short survey was developed, but is not validated. Because the initial assessment sought to look for a change from before to after the workshop, it is acceptable. Instead of asking students to rate their knowledge and experience, a written quiz could have been administered to grade their knowledge. A numerical estimation could have been gathered from participants or patient logs to gauge experience. In this study, the survey was administered at the end of the workshop, filling before and after responses simultaneously. This could lead to data bias in that the workshop experience could have altered participants’ actual entry response. For example, a participant could have realized how much they did not know before or concluded this was repetition.
Although this workshop fits the definition of educators and learners from two or more professions working together, the goal of the initial workshop was primarily skill-based with reference to future referrals. The overlying goal was to encourage a better understanding of optometry and to help with the referral process discussion at the next workshop. Actual integration of the classroom with students of both disciplines would be difficult for this subject matter due to the fact that the two disciplines require a different level of depth of understanding of the material. Additionally, in the case of MCPHS University, the size of the physician assistant program is much larger than the optometry program. Therefore, accommodating both programs would require space for approximately 190 students. At the time of this workshop, the inaugural class of optometry students had not begun anterior segment evaluation in their curriculum. Taking that into consideration, upper-level optometry students could be utilized in future workshops as patients or mentors.
The current PA seminar program has multiple sessions throughout the year, which allows for different optometric topics at each. Mastery of skills such as drop instillation is much easier to accomplish in a single workshop. Slit-lamp examination, on the other hand, is a skill that takes time to develop and may be best introduced and reviewed in a format of multiple workshops. The intended direction is toward progressive programs that transition from didactic to technical/laboratory and ultimately to clinical/integrative. This correlated with other suggested formats.8 It would also be beneficial to incorporate the PA program into the teaching component of the optometry program for vital signs, including blood pressure measurement, cranial nerve assessment or injections.
Conclusion
Overall, the workshop was successful and enjoyed by both the students and the faculty. The relevance and format were appropriate and could be used for these topics or other topics in the future. The survey data showed a significant increase in knowledge and experience level with each topic and technique. Although this was an initial pilot, it provided a foundation from which to build future workshop programs.
The goals for future programs include:
1) Having the optometry program conduct the introductory lectures in the physician assistant didactic year
2) Utilizing a validated survey, such as the Readiness for Interprofessional Learning Scale (RIPLS),10 to determine student readiness for IPE
3) Posting review content prior to the workshops to maximize hands-on time
4) Developing and implementing a pre-workshop quiz to better assess entry-level knowledge
5) Developing and implementing a post-workshop quiz that could be done immediately after the workshop (Another quiz could also be given later in the curriculum to assess retention.)
6) Modifying the physician assistant program patient logs to tally eye-related procedures to more accurately monitor actual clinical experience
7) Developing and implementing a proficiency exam to ensure technical aptitude
8) Exploring areas in the optometry program that could be taught by physician assistant program faculty
9) Developing communication strategies to discuss pertinent findings between professions
10) Adapting the curriculum in both programs to bring students together to discuss patient care, referral process and how they can manage patients together.
References
1. Centre for the Advancement of Interprofessional Education (Website) Fareham, United Kingdom; c2014. Available: https://caipe.org.uk/resources/defining-ipe/.
2. World Health Organization (WHO). Framework for action on interprofessional education and collaborative practice. Geneva: World Health Organization. 2010.
3. Interprofessional Education Collaborative Expert Panel. Core competencies for interprofessional collaborative practice: Report of an expert panel. Interprofessional Education Collaborative. 2011.
4. Oandasan I, Reeves S. Key elements of interprofessional education. Part 1: The learner, the educator, and the learning context. J of Interprofessional Care. 2005;1:21-38.
5. Oandasan I, Reeves S. Key elements of interprofessional education. Part 2: Factors, processes, and outcomes. J of Interprofessional Care. 2005;1:39-48.
6. Reeves S, Zwarenstein M, Goldman J, Barr H, Freeth D, Hammick M, Koppel I. Interprofessional education: effects on professional practice and health outcomes. Cochrane Database of Systemic Reviews. 2008. Issue 1. Art No.: CD002213. DOI: 10.1002/14651858.CD002213,pub2.
7. Luplow D. Michigan College of Optometry Interprofessional Wellness Clinic: Focus on Diabetes. Health and Interprofessional Practice. 2012. 1(2):eP1021.
8. Aston SJ, Rheault W, Arenson C, Tappert SK, Stoecker J, Orzoff J, Galitcki H, Mackintosh S. Interprofessional Education: A review and analysis of programs from three academic health centers. Acad Med. 2012;87:949-955.
9. Sheppard KD, Ford CR, Sawyer P, Foley KT, Harada CN, Brown CJ, Ritchie CS. The interprofessional clinical experience: interprofessional education in the nursing home. J of Interprofessional Care. 2014. Online Art No.: 1469-9567. DOI 10.3109/13561820.2014.942776.
10. Parsell G, Bligh J. The development of a questionnaire to assess the readiness of health care students for interprofessional learning (RIPLS). Medical Education. 1999;33:95-100.



