Topiramate-Induced Acute Bilateral Angle Closure Glaucoma and Transient Myopia
Vanessa Santos-Nevarez OD, Jenette Cantrell OD, FAAO, Paul Gruosso OD, Joseph Miller OD, FAAO, Tina Culotta-Glynn DO
Abstract
Topiramate is an oral medication used in the treatment of epilepsy and prevention of migraines. It also has several off-label uses, including treatment of alcoholism and substance dependence. Topiramate and other sulfa-derived medications have been associated with secondary acute angle closure and myopic shift. This case report demonstrates the role of the optometrist as part of an interdisciplinary team in the management of an episode of acute bilateral angle closure. It also illustrates the importance of a team approach to treating patients as a whole for their general well-being.
Key Words: topiramate, bilateral angle closure, secondary angle closure, myopic shift
Background
Topiramate is a sulfamate-substituted monosaccharide used in the treatment of epilepsy and migraines.1 It also has an off-label use in the treatment of bipolar disorder, depression and as a weight reduction agent, among other uses.2 With the growing off-label use of this oral medication, it is important to raise awareness within the medical community of the potentially blinding side effects of topiramate. We describe a case of a 34-year-old white male who presented to the emergency department with complaints of sudden onset bilateral vision loss and headaches after doubling the dose of topiramate and the role of an interdisciplinary team in the patient’s care. This case is intended to demonstrate the role of an interdisciplinary team in maximizing patient care and the optometrist’s contribution in educating fellow healthcare providers of the side effects of this widely used oral medication. This case is appropriate for more advanced optometry students who have had pharmacology courses and patient care experience. At most colleges, it would be geared toward optometry students at the end of their third year and all fourth-year students.
Case Description
A 34-year-old Caucasian male presented to the emergency room with complaints of blurry vision, itchiness and tearing in both eyes with an associated headache that occurred two hours after awakening. General and neurologic assessment at the emergency room was unremarkable. Due to the possibility of a cerebrovascular accident (CVA), computed tomography (CT) imaging of the head was ordered. The results were negative for a CVA. The optometry department was contacted for discussion of the case. We discussed the history and findings with the emergency room physician and recommended the patient be seen in the optometry department for further evaluation.
The patient presented to our eye clinic with complaints of acute progressive decreased vision,
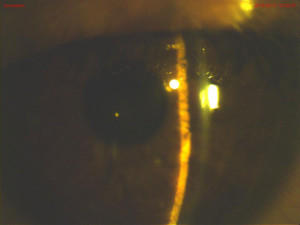 |
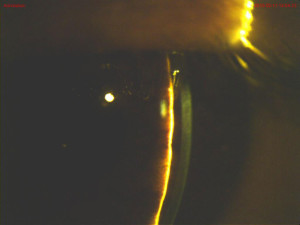
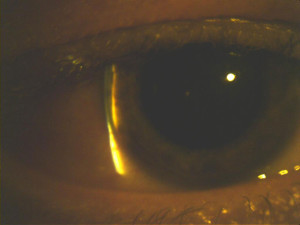
foreign body sensation, pain over both eyes and an associated frontal headache. The foreign body sensation was relieved by the use of preservative-free artificial tears every 2 hours in both eyes and the headache was now resolved. The patient denied pain, photophobia and redness in either eye. The patient had no past ocular history and had never worn glasses. Social history was remarkable for anxiety, alcohol, benzodiazepine and illicit substance abuse. The patient was enrolled in a substance abuse treatment program and had recently undergone several changes in the treatment of the above conditions under the care of the psychiatry department. His medication list included suboxone 4 mg sublingual for opioid dependence, trazodone 150 mg by mouth at bedtime for sleep and topiramate 25 mg by mouth twice daily as off-label treatment for anxiety and dependence symptoms. The patient had been on suboxone and trazodone for 4 months without complications and had begun taking topiramate 10 days prior to our encounter. He reported doubling the dose of topiramate from 50 mg to 100 mg on the night prior to the onset of the symptoms in an attempt to control his anxiety and craving symptoms. The examination findings are listed in Table 1. (Figures 1A, 1B, 2A, 2B)
Findings key to a diagnosis were bilateral narrowing of the angle structures, increased intraocular pressure and myopic shift. All are indicative of angle closure secondary to ingestion of topiramate. The case was reviewed with the ophthalmology team. We discussed the patient’s chief complaint and findings and reviewed the patient’s medical history including his current medication list. The ophthalmology team evaluated the patient and agreed with our findings. We discussed the management of the case and performed a unilateral trial of tropicamide 1% ophthalmic solution in the right eye. Slit lamp examination of the right eye 4 hours later revealed a deeper anterior chamber depth than previously noted, with no improvement in the left eye anterior chamber depth. The intraocular pressure was 24 mmHg in the right eye and 22 mmHg in the left eye at the time. The psychiatry department was notified of the case, and it was agreed that the patient should discontinue topiramate with follow-up at their clinic once the ocular findings resolved. The patient was given acetazolamide 250 mg by mouth and tropicamide 1% ophthalmic solution for the left eye and sent home with an appointment for follow-up the next day.
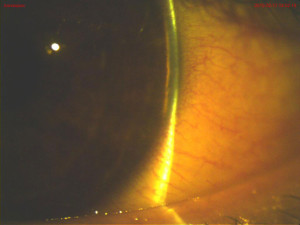
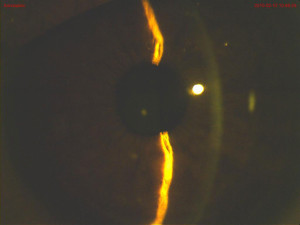
At the follow-up exam the patient reported improved vision and resolved eye pain. The uncorrected visual acuity was unchanged at 20/50 in the right eye and improved to 20/100 in the left eye. The vision was correctable to 20/20 in each eye with a decrease in myopia in the refraction, measuring -2.00D sphere in the right eye and -2.75D sphere in the left. Slit lamp examination revealed slight bowing of the iris and improved chemosis in each eye. The anterior chamber was deeper in the right eye compared to the left eye, Von Herrick grade 4 and 3 respectively. (Figures 3 and 4) Gonioscopy of both eyes revealed ciliary body band with a steep iris approach in all angles. At the one-week follow-up, the patient reported resolution of symptoms and normal vision. The uncorrected visual acuity was 20/20 in each eye, intraocular pressure was 14mmHg in each eye and slit lamp findings were unremarkable with deep and quiet anterior chambers and resolution of conjunctival chemosis.
A few weeks later the patient had a follow up visit with the psychiatry department for a re-evaluation after discontinuing topiramate. The patient reported improvement of his anxiety and substance abuse while on suboxone and trazadone only. The patient was doing well without topiramate treatment, had found a job, was sleeping well and reported mild alcohol use and no use of illicit substances. No further medications were recommended at the time.
Education Guidelines
Learning objectives
1. understand the role of the optometrist in an interdisciplinary setting
2. describe the signs and symptoms of secondary acute angle closure from topiramate
3. understand treatment and management of primary acute angle closure and secondary angle closure from topiramate
4. describe the physiological mechanism of action for the cause of symptoms
5. identify key diagnostic tests for an adverse reaction of topiramate
Key concepts
1. topiramate, used primarily in the treatment of migraine, can induce an ocular adverse reaction resulting in bilateral secondary acute angle closure and myopic shift
2. treatment for topiramate-induced acute angle closure differs from that of primary angle closure
3. ultrasound biomicroscopy and optical coherence tomography are useful tools in the monitoring of signs and symptoms
4. discontinuation of the medication, use of cycloplegic drops and intraocular pressure-lowering medications result in resolution of symptoms
Discussion points
1. describe and identify normal anatomy of the angle
2. signs and symptoms of acute angle closure
3. difference between primary angle glaucoma and acute angle closure
4. ocular side effects of systemic medications
5. systemic medications that can lead to angle closure
Literature review
Topiramate (Topamax, Ortho McNeal Pharmaceuticals, Raritan NJ), a sulfamate-substituted monosaccharide, was first approved by the FDA in 1996 for the treatment of epilepsy. In 2004 it received additional approval for the prevention of migraine headaches in adults.1 Off-label uses for topiramate include weight reduction, bipolar disorder, depression and neuropathic pain.2 In the mechanism of action for the relief of migraine headaches, topiramate acts as an enhancer for neurotransmitter y-aminobutyric acid (GABA) activity, antagonizer for a-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid-kainate and sodium and calcium channel blocker, resulting in decreased neurotransmission, hyperexcitability and migraine headaches.1
Numerous case reports have associated anti-depressive medications and sulfa-derived drugs such as topiramate with a myopic shift and secondary acute angle closure.2-8 There is approximately a 3% risk of developing an adverse reaction to a sulfonamide.3 The first case report of an association of symptoms with the use of topiramate was published by Banta et al. in 2001. Subsequently, Ortho McNeal Pharmaceuticals circulated a letter indicating the reported adverse reactions of the drug. It is hypothesized that ciliochoroidal effusion and ciliary body edema cause forward rotation of the ciliary body and forward displacement of the iris-lens diaphragm, resulting in anterior chamber shallowing, myopic shift and
increased intraocular pressure.4-6 The mechanism of action of topiramate resulting in choroidal effusion is not well understood at this time, although its weak carbonic anhydrase inhibitor activity, elevated prostaglandin levels 5 and changes in membrane potential leading to fluid movement could be implicated.7 The mechanism for acute myopia is the forward displacement of the lens, although it had been proposed that lens thickness changes are also responsible for the acute myopia. Lens thickness changes contribute to only 9-16% of cases of shallowing of the angle, with choroidal effusions being responsible for most of the decrease in anterior chamber depth.8 While some reports have postulated that the small changes in lens thickness are due to lens osmotic changes, other reports indicate that the changes in lens thickness are due to reduction of zonular tension from the choroidal effusion4 displacing the lens-iris diaphragm forward.8 The symptoms can occur without predilection in any patient, even in the absence of anatomic predisposing factors for acute angle closure. Therefore, ocular examination prior to beginning topiramate therapy would not identify eyes at risk of developing symptoms.
Primary acute angle-closure glaucoma and topiramate-induced secondary angle-closure glaucoma have some signs and symptoms in common, such as conjunctival hyperemia, corneal edema, shallowing of the anterior chamber, elevated intraocular pressure and visual defects, and without proper management, blindness. Careful history and examination are essential in differentiating the two conditions given the marked difference in management for each. The onset of topiramate-induced angle closure is acute, with most cases occurring in the first 2 weeks of initiation of treatment as well as within 6 hours of doubling the dose.9 The symptoms of acute myopia may present after only a few hours of ingestion and may take several weeks to fully resolve. A reported mean age of 34 has been found, and an association with various doses ranging from 50-100 mg has been found, with about 50% of cases occurring in doses of 50 mg or less. Up to 89% of cases have been reported to occur mostly in females.10 Other associated symptoms that have been reported include blepharospasm, myokymia, oculogyric crisis, periocular edema, paresthesia, periocular pain, scleritis, nystagmus and, with large doses, diplopia.9 Reports have also associated reversible macular striae at the level of the internal limiting membrane, which could also be caused by vitreomacular traction or choroidal effusion.11 Recent reports have associated visual field defects without the presence of elevated intraocular pressure with the use of topiramate.12
Diagnostic tools such as gonioscopy and B-scan aid in visualizing the angle structures and choroidal effusion respectively, with ultrasound biomicroscopy being one of the most available tools for providing high-resolution imaging of the anatomy for confirmation of ciliochoroidal effusion as the etiology for secondary angle closure.13, 14 Anterior segment optical coherence tomography is an effective non-invasive method for the evaluation and monitoring of angle closure, effusion and rotation of the ciliary body.15,16
Treatment consists of immediate discontinuation of topiramate therapy in concert with the prescribing physician because dosing changes of at least 50 mg could have systemic complications.9 Administration of cycloplegic agents lowers the intraocular pressure by retraction of the ciliary body. Topical and oral intraocular pressure-lowering agents are indicated. Peripheral iridotomy is not indicated in drug-induced secondary angle closure because the mechanism of action is not that of pupillary block and it would be of no therapeutic value.4 Pilocarpine is contraindicated as it may cause further displacement of the lens-iris diagram and possibly precipitate a relative pupillary block.17 Topical steroids may prove to be beneficial to reduce choroidal effusion by stabilizing cell membranes.
Discussion
The patient’s initial complaints of sudden bilateral blurred vision and headaches at the emergency department generated a list of differential diagnoses too numerous to name. A detailed history and further examination were needed. As part of the integrated setting of a hospital, an interdisciplinary team of specialty services can be brought to work together to facilitate the patient’s care. The optometrist played an important role as the primary eyecare provider in the care of this patient. Consultation from the emergency room physician directly with the optometrist for discussion of the case ensured adequate assessment of the ocular health and was essential for the delivery of prompt management and treatment.
Detailed history and review of systems played a vital part in finding the etiology for the patient’s symptoms. During the initial optometric examination, the patient reported progressive blurry vision along with foreign body sensation that was relieved by the use of artificial tears. The patient reported excellent vision without spectacles prior to this episode. He also reported frontal headaches and a headache-like feeling over his orbit and brow. Entrance vision testing revealed decreased uncorrected vision in both eyes that was correctable to 20/20 with a significant myopic shift in each eye. Which conditions could result in a bilateral shift in refractive error? The main differential diagnosis with this initial information would be refractive shift due to uncontrolled diabetes. Slit lamp examination was remarkable for edematous lids, conjunctival chemosis and injection, shallow anterior chamber depth, forward bowing of the iris and narrow Von Herrick angle evaluation. The differential diagnoses included CVA, migraine headache, angle-closure glaucoma and choroidal effusion syndrome. Which other problem-focused testing could be performed to narrow down the differential diagnosis? Given the appearance of the angle structures, measurement of intraocular pressure and gonioscopy were warranted. Tonometry revealed moderately elevated intraocular pressures in both eyes.
Four-mirror gonioscopy revealed a convex iris approach and no visible angle structures in either eye. This appeared to be an atypical case of angle closure. What are the different types of angle closure? Which key elements differentiate the different classifications?
Primary acute angle closure typically presents in an older population, with the highest incidence between 55-65 years old.18 It is more common in Southeast Asians, Chinese and Eskimos. In Caucasians, it accounts for approximately 6% of all glaucomas and affects 1:1000 over age 40. Females are affected 3 to 4 times more than males. Risk factors include hyperopia and short axial length. Signs and symptoms include blurry vision, hazy cornea, mid-dilated pupil, shallow anterior chamber, elevated intraocular pressure, vomiting, nausea and narrow and occludable angles on gonioscopy. Our patient presented with a clear corneal appearance and normal pupillary reaction, and his refraction revealed a bilateral myopic shift rather than a hyperopic refractive error. Therefore primary angle closure is unlikely in this case. Secondary angle-closure glaucoma can have several etiologies, including being medication-induced. A complete review of secondary glaucoma is beyond the scope of this paper. In the case of bilateral acute angle closure and myopic shift, drug-induced etiologies should be considered in the differential diagnosis.
Review of the medical history and critical thinking analysis of the pertinent findings were crucial in identifying the key elements in this case to make a diagnosis. Access to electronic medical records played a major part by providing additional information to guide in the search of the causative agent. The patient’s record did not indicate a diagnosis of diabetes; therefore, a diabetic refractive error shift was unlikely. Review of the patient’s history and medications revealed a significant history and treatment for anxiety, alcohol and substance dependence by the psychiatry department. The patient was also enrolled in a substance abuse treatment program at our facility as an adjunct to medical therapy. The patient had undergone several changes in his medical treatment for the management of anxiety without much success. A recent change included the addition of topiramate for off-label treatment of anxiety and cravings of alcohol and illicit substances.
Alcohol and substance abuse disorders have a significant impact on the nation’s health, economy and welfare. In 2013, approximately 7% of adults in the United States age 18 and older had an alcohol use disorder ,19 a medical term for a severe drinking problem, and 9.4% of persons age 12 and older reported the use of illicit drugs.20 The annual cost of health care for alcoholism and illicit drug use in the United States totals $25 billion and $11 billion respectively.21 In 2013, 8.6% of persons age 12 or older needed treatment for alcohol or illicit drug use, and only 0.9% of those received treatment at a substance abuse treatment facility.Treatment for alcohol and substance abuse consists of medication therapy and behavioral therapy. There are limited pharmacologic agents for treating alcohol dependence, with only three approved by the U.S. Food and Drug Administration: naltrexone, acamprosate and disulfiram. Clinical trials of topiramate have shown improvement in alcohol dependence and withdrawal symptoms, increasing the popularity of its off-label use. There is limited data on the use of topiramate for the treatment of substance abuse.22, 23
Alcohol and substance abuse treatment programs are an integral part of patients’ success in overcoming dependencies. The optometry department is often involved in the care of these patients to assess their visual needs as their treatment includes classes geared toward rehabilitation back into the community. Ocular symptoms from medications, such as blurriness and diplopia, as well as an increase in visual demands and need for glasses are the major concerns presented at the time of the encounter. The initial ocular assessment should include a comprehensive history and a review of systemic history including current medications. Patients should be educated on their ocular health status and on the possible visual symptoms and ocular sequelae they might encounter in the course of their medical treatment. Communication with the psychologist, psychiatrist and therapist is essential due to the increase of off-label use of topiramate and the potentially devastating ocular complications, which can hinder patients’ progress and success in the rehabilitation program.
In our case, the patient reported doubling of the dose of topiramate, a sulfamate-derived medication that has been linked to myopic shifts and forward rotation of the iris-lens diaphragm, prior to the onset of ocular symptoms. Once the causative agent was identified, co-management of the patient’s care with an interdisciplinary team led to the discontinuation of the medication and proper ocular management. This resulted in resolution of the patient’s symptoms and prevention of irreversible blindness.
Counseling of patients and their prescribing providers on the potentially blinding side effects of topiramate has become of growing importance due to the widespread off-label use of this medication. Members of the interdisciplinary team that participated in this patient’s care consisted of the emergency department physician whom the patient presented to for assessment of overall health during the acute episode, the psychiatry and pharmacy departments for the ongoing management of the alcohol and substance abuse disorder, and optometry in concert with ophthalmology for treatment and management of the ocular symptoms.
Discontinuation of topiramate should be managed in conjunction with members of the interdisciplinary team due to the detrimental side effects that can occur with sudden discontinuation of the medication. An additional service that could have a significant impact on a patient’s progress would be the psychology department, which could offer counseling for coping with transient vision loss and exacerbation of anxiety symptoms throughout the acute episode. Optometry should continue to monitor the ocular signs and symptoms throughout a patient’s care.
Conclusion
Ocular complications from topiramate therapy appear to be rare, but with the growing popularity of the medication and frequent off-label use, it is important to create awareness among patients and healthcare providers of the possible drug-induced ocular sequelae and the importance of seeking care for appropriate treatment and follow-up. Communication and teamwork within the interdisciplinary team are important to facilitate timely care for patients. The role of the optometrist as the first point of contact and primary eyecare provider for this patient’s ocular symptoms was essential in the management and eventual resolution of this patient’s acute episode of bilateral secondary angle-closure glaucoma.
Acknowledgement
Imaging by Steve Derr
References
1. Wenzel RG, Schwarz K, Padiyara RS. Topiramate for migraine prevention. Pharmacotherapy. 2006;26(3):375-87.
2. Gawley SD. Topiramate induced acute transient myopia: a case report. Cases J. 2009;2:7430.
3. Panday VA, Rhee DJ. Review of sulfonamide-induced acute myopia and acute bilateral angle-closure glaucoma. Comp Ophthalmol Update. 2007;8(5):271-6.
4. Banta JT, Hoffman K, Budenz DL, Ceballos E, Greenfield DS. Presumed topiramate-induced bilateral acute angle-closure glaucoma. Am J Ophthalmol. 2001;132(1):112-4.
5. Rhee DJ, Goldberg MJ, Parrish RK. Bilateral angle-closure glaucoma and ciliary body swelling from topiramate. Arch Ophthalmol. 2001;119:1721-3.
6. Boentert M, Aretz H, Ludemann P. Acute myopia and angle-closure glaucoma induced by topiramate. Neurology. 2003;61(9):1306.
7. Levy J, Yagev R, Petrova A, Lifshitz T. Topiramate-induced bilateral angle-closure glaucoma. Can J Ophthalmol. 2006;41:221-5.
8. Craig JE, Ong TJ, Louis DL, Wells JM. Mechanism of topiramate-induced acute-onset myopia and angle closure glaucoma. Am J Ophthalmol. 2004;137:193-5.
9. Fraunfelder FW, Fraunfelder FT, Keates EU. Topiramate-associated acute, bilateral, secondary angle-closure glaucoma. Ophthalmology. 2004;111:109-11.
10. Thambi L, Kapcala LP, Chambers W, Nourjah P, Beitz J, Chen M, Lu S. Topiramate-associated secondary angle-closure glaucoma: a case series. Arch Ophthalmol. 2002;120:1108.
11. Natesh S, Rajashekhara SK, Rao AS, Shetty B. Topiramate-induced angle closure with acute myopia, macular striae. Oman J Ophthalmol. 2010;3:26-8.
12. U.S Department of Health and Human Services: U.S Food and Drug Administration. Available from: https://www.fda.gov/Safety/MedWatch/SafetyInformation/ucm195797.htm.
13. Saffra N, Smith SN, Seidman CJ. Topiramate-induced refractive change and angle closure glaucoma and its ultrasound bimicroscopy findings. BMJ Case Rep. 2012;10:1136.
14. Abtahi MA, Abtahi SH, Fazel F, Roomizadeh P, Etemadifar M, Jenab K, Akbari M. Topiramate and the vision: a systematic review. Clin Ophthalmol. 2012;6:117-131.
15. Van Issum C, Mavrakanas N, Schutz JS, Shaarawy T. Topiramate-induced acute bilateral angle closure and myopia: pathophysiology and treatment controversies. Eur J Ophthalmol. 2011;21(4):404-9.
16. Palomares P, Anselem L, Diaz-Llopis M. Optical coherence tomography for diagnosis and monitoring of angle-closure glaucoma induced by topiramate. Can J Ophthalm. 2007;42(4):633-4.
17. Medeiros FA, Zhang XY, Bernd AS, Weinreb RN. Angle-closure glaucoma associated with ciliary body detachment in patients using topiramate. Arch Ophthalmol. 2003;121(2):282-5.
18. Rhee, DJ. Glaucoma: Color Atlas and Synopsis of Clinical Ophthalmology (Wills Eye Series) New York: McGraw-Hill, Inc.; 2003.
19. National Institute on Alcohol Abuse and Alcoholism. Alcohol facts and statistics. [Internet] Bethesda (MD): National Institutes of Health; [updated 2015 March; cited 2015 March 1] Available from: https://www.niaaa.nih.gov/alcohol-health/overview-alcohol-consumption/alcohol-facts-and-statistics.
20. Substance Abuse and Mental Health Services Administration, Results from the 2013 National Survey on Drug Use and Health: Summary of National Findings, NSDUH Series H-48, HHS Publication No.(SMA) 14-4863. Rockville, MD: Substance Abuse and Mental Health Services Administration, 2014.
21. National Institute on Drug Abuse. Drug Facts: Nationwide Trends. [Internet] Bethesda (MD): National Institutes of Health; [updated 2015 January; cited 2015 March 1] Available from: https://www.drugabuse.gov/publications/drugfacts/nationwide-trends.
22. Kenna GA, Lomastro TL, Schiesl A, Leggio L, Swift RM. Review of topiramate: an antiepileptic for the treatment of alcohol dependence. Curr Drug Abuse Rev. 2009;2(2):135-42.
23. Shinn AK, Greenfield SF. Topiramate in the treatment of substance-related disorders: a critical review of the literature. J Clin Psychiatry. 2010;71(5):634-48.