PEER REVIEWED
Transient Vision Loss
Stephanie Uchida OD, Haley Wilson OD, Jonathan Goodwin OD, Ashley Toland OD, FAAO, and Tina R. Porzukowiak, OD, FAAO, Dipl.
Abstract
Transient vision loss (TVL) is a common symptom presenting to eyecare providers. The differential diagnosis of TVL ranges from benign to emergent life- or sight-threatening conditions. A thorough case history and ocular examination directs the physician to the most likely etiology. The purpose of this teaching case report is to guide optometric students and residents in the clinical approach and management of this condition.
Key Words: amaurosis fugax, stroke, transient ischemic attack, transient visual loss, transient vision loss, transient visual obscurations
Background
Transient vision loss is the acute loss of vision, either monocular or binocular, lasting less than 24 hours.1 The potential etiologies are wide-ranging, and many are ocular or systemic emergencies. A thorough case history and attention to patient demographics is key. Clarifying the laterality, duration, pattern of loss and recovery, associated visual and systemic symptoms, provoking factors, patient age and personal and family health history can guide the physician to an accurate diagnosis. The ocular examination can reveal the direct cause (as in retinal embolus), but in some cases the exam may be normal. Determining the most likely cause of vision loss directs further evaluation and treatment to preserve vision and overall health.1,2
Transient vision loss is a common symptom presenting to eyecare providers. Its evaluation, treatment and management are learned skills. The target audience for this teaching case report is optometric educators with the targeted learner being third- or fourth-year optometry students and optometric residents.
Student Discussion Guide
Case description
A 70-year-old Black male presented for an emergency eye examination with the complaint of acute, recurrent, transient vision loss of the right eye (OD) presenting as gradual dimming and inferior altitudinal visual field loss with associated angina pectoris. The first episode occurred 6 months prior to the visit and recurred monthly with a duration of 5 minutes. The vision loss was not gaze-evoked or associated with photostress, Valsalva maneuver or postural change. The patient denied confusion, fever, focal weakness, dysarthria, emesis, headache, intracranial noises, malaise, nausea, neck pain, phonophobia, photophobia, photopsia, presyncope, Raynaud phenomenon, scalp tenderness, tinnitus or visual aura.
Ocular history was remarkable for dry eye syndrome and pseudophakia in both eyes (OU). Medical history was significant for aortic regurgitation, constipation, depression, eczema, erectile dysfunction, hyperlipidemia, hypertension, low testosterone, malignant prostate neoplasm (in remission), osteoarthritis, polysubstance abuse (in remission), thyroid nodule and vitamin D deficiency. Medications included bupropion (Wellbutrin XL, Teva Pharmaceuticals), vitamin D3 (cholecalciferol, Polymed Therapeutics), hydrochlorothiazide (Microzide, Allergan), loratadine (Claritin, Schering-Plough), polyethylene glycol 3350 oral powder (Miralax, Bayer Healthcare), sildenafil citrate (Viagra, Pfizer), simvastatin (Zocor, Merck) and testosterone intramuscular injections (Delatestryl, Endo Pharmaceuticals). The patient reported no known drug allergies. Family history was positive for coronary artery disease in the mother. He described a history of tobacco use, occasional alcohol intake and daily marijuana use. He was oriented to person, place and time; his mood was appropriate.
Best-corrected distance visual acuities were 20/20- OD and 20/20 left eye (OS). Pupils were equally round and reactive to light without an afferent pupillary defect. Extraocular muscles were smooth and full OU. Confrontation visual fields were full to finger counting OD, OS. Near cover test was orthophoric. Slit lamp examination revealed normal adnexa, lids, lashes, sclera, conjunctiva, cornea, anterior chamber and iris OD, OS. The posterior chamber intraocular lenses were well-centered and clear OD, OS. Goldmann applanation tonometry measured intraocular pressures of 17 mmHg OD and 18 mmHg OS at 9:37 a.m. Dilated funduscopic examination revealed normal optic nerve (cup-to-disc ratio 0.30/0.30), macula, vitreous, choroid and retinal periphery OD, OS. Vessels were mildly torturous and attenuated with no evidence of retinal emboli OD, OS.
The patient was diagnosed with recurrent transient vision loss OD with associated angina of unknown etiology and advised to report to the emergency department for STAT physical evaluation and initiation of a stroke protocol. A phone call was made to the emergency department, and eye exam results were forwarded for review.

Figure 1. CTA head and neck sagittal profile demonstrating a right carotid artery bulb cholesterol plaque (red arrow).
Click to enlarge
In the emergency department, presenting vital signs included temperature 97.4° F, pulse 65 bpm, respiratory rate 16, blood pressure 120/73, pulse oximetry 98% and chest pain scale 5/10. Echocardiogram revealed sinus bradycardia of 54 bpm. Complete blood cell count was consistent with anemia. Comprehensive metabolic panel, hemoglobin A1c, prothrombin time, partial prothrombin time, international normalized ratio, Westergren erythrocyte sedimentation rate, C-reactive protein, troponin I and urinalysis were normal. Computed tomography (CT) of the head with contrast revealed microvascular ischemic disease of the brain. Computed tomography angiography (CTA) of the head and neck showed atherosclerotic plaque at the right carotid bifurcation extending to the right carotid bulb and proximal internal carotid artery contributing to approximately 60% narrowing of the vessel as seen in Figure 1. The left side showed similar findings with approximately 50% stenosis. Chest CT with contrast revealed moderate to severe coronary atherosclerosis. Magnetic resonance imaging (MRI) of the brain with and without contrast using diffusion weighted imaging was negative for stroke. Neurology evaluation confirmed a transient ischemic attack (TIA) causing amaurosis fugax of the right eye. The patient was discharged on aspirin 81 mg daily and advised to continue all current medications. After communication of exam findings, outpatient bilateral carotid artery duplex (a.k.a. Doppler ultrasound) was coordinated with primary care within 2 weeks. Eye clinic follow-up was scheduled for 1 month. Neurology instructed that a vascular surgery consultation should be considered pending carotid duplex results.
Educator’s Guide
The educator’s guide includes the necessary information for teaching and discussing the case.
Key concepts
- Recognizing clinical symptoms and the importance of a detailed history
- Specifying the differential diagnoses of TVL
- Developing management strategies to work through differential diagnoses
- Understanding timely referral to the emergency department and other specialists
Learning objectives
Upon conclusion of this case, participants should be able to:
- Describe the diagnostic criteria of TVL
- Differentiate TVL from other vision disturbances
- Review visual pathway and its relationship to the nature and features of TVL
- Recommend and understand the appropriate additional diagnostic tests
- Develop an interprofessional collaborative treatment plan for emergent evaluation
Discussion questions
1. Knowledge, concepts, facts and information required for critical review of the case
a. How does the patient’s systemic health play a role in the ocular diagnosis?
b. Does the patient fit the typical demographics of TVL?
c. What are the history of present illness (HPI) elements that help differentiate TVL from other forms of temporary vision loss (e.g., transient vision obscurations, uncontrolled dry eye syndrome?
d. What other providers need to be included as part of an interprofessional care team?
2. Differential diagnosis
a. What is the differential diagnosis of TVL after case history and after the ocular exam?
b. What tests should be performed to narrow the differential diagnosis?
c. What further testing may be needed pending the results of the initial studies?
3. Patient management and the role of the optometrist
a. What treatment/management would be most appropriate for the patient medically and regarding lifestyle changes?
b. How quickly should the patient undergo laboratory and imaging studies?
c. How should the patient be managed after test results are obtained?
d. How soon should a patient be seen for an eye examination with TVL symptoms?
e. Should TVL always be managed in an emergent manner?
f. How might the provider manage this case differently?
4. Critical-thinking concepts
a. In the case described, what aspects of the patient’s health history were important in determining the underlying etiology?
b. What were some of the distinguishing features of the patient’s TVL that helped guide the workup?
Learning assessment
Teaching instructions and assessment methodology can include:
-
- Knowledge base of the pertinent case history questions can be tested through verbal discussion or listing.
- Knowledge base of the differential diagnosis can be tested through table development comparing and contrasting characteristics of varying etiologies.
- Critical-thinking skills can be expanded via review of other published TVL-specific case reports.
- Management skills can be assessed by creating various case scenarios with differing serology and imaging results.
- The purpose of this case report is to help clinical novices critically review the case history and clinical findings consistent with TVL and to develop management strategies. A faculty member or teaching assistant could lead a discussion of the case presentation in either a large classroom setting or small group. In a larger setting, real-time audience polling can monitor student comprehension. During the discussion, students should be given the initial case presentation in a stepwise fashion (i.e., history, clinical findings, serology results, vascular imaging reports, neuroimaging studies). This enables the learner to critically think through the presentation and differential diagnosis. Following the discussion, management strategies including collaboration with other medical professionals can be reviewed. It is important for the discussion to review the various differential diagnoses and how the management strategy and referrals change depending on the case history and examination findings.
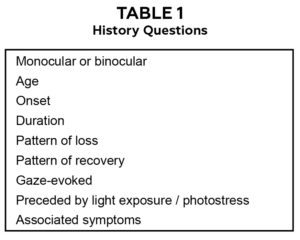
Table 1. Click to enlarge

Table 2 Click to enlarge
Discussion
Etiology
Disease at any level in the visual pathway can result in temporary vision loss. However, disease to structures that refract light such as the cornea and ocular media typically do not result in complete loss of vision as light can still stimulate the retina. Disease to the retina, optic nerves, optic radiations or visual cortex can cause more explicit vision loss. This overt TVL most often stems from transient vascular compromise to the eye or afferent visual pathway in the brain. A disruption in blood flow to the retina or occipital lobe, from ischemia or vascular insufficiency whether hemodynamic or embolic, can result in a dark curtain of vision loss in one or both eyes lasting up to 30 minutes.3 Perfusion of the optic nerve and retina are also dependent on intracranial pressure. When intracranial pressure is increased, as in papilledema, simultaneous transient monocular or binocular vision obscurations that last less than 10 seconds can occur.4 To assist in finding the etiology of TVL, Table 1 highlights important questions to ask when gathering the ocular history. Staff may find it helpful for phone triaging. Table 2 focuses on the TVL-associated symptoms serving to further refine the differential diagnosis.
Clinical features
Patients presenting with TVL often have an unremarkable eye examination; however, ocular findings help point to an etiology and differentiate true TVL from other vision disturbances. The following paragraphs highlight the most common ocular considerations.
Dry eye syndrome, corneal erosion and corneal hydrops are known to cause vision fluctuations especially with blinking and eye-drop instillation.5
Hyphema, including uveitis-glaucoma-hyphema syndrome, can present with gradual, diffuse “misting” of vision and slow recovery.
Subacute angle-closure attacks cause intermittent temporary vision loss from corneal edema.
Pupil abnormalities accompanying TVL increase suspicion for optic nerve or neurological disease. Ipsilateral Horner syndrome accompanied with facial or neck pain warrants emergent evaluation for carotid dissection.6
Gaze-evoked TVL may be elicited by having the patient move the eyes and hold each position of gaze for 5 seconds with the examiner noting any change in vision function or pupil activity. Orbital disease can produce a gaze-evoked monocular TVL especially in downgaze with reading.
Dilated examination is essential to evaluate for optic nerve anomalies, retinal emboli or vascular occlusive disease. Patients with carotid and cardiovascular disease are at high risk for retinal emboli. Emboli are primarily composed of either cholesterol, which makes them refractile and gold in appearance, or a combination of platelets and fibrin, which form longer grey-white plugs that fill the vessel lumen.5 Calcium emboli, which are chalky white, globular and often near the optic disc, come from calcified heart valves.6
Ocular ischemic syndrome (OIS) is characterized by mid-peripheral dot-and-blot hemorrhages and may cause monocular TVL, particularly with exposure to bright light known as photostress. Venous stasis retinopathy, as seen in OIS, is associated with a vascular occlusion anywhere from the heart to the eye. Sludging of conjunctival vessels is a subtle anterior segment finding in which small areas of blood pooling are evident with red-free light due to vascular impedance.7
Optic nerve edema, optic neuritis, papilledema or other disorders disrupting the anatomy of the optic nerve can cause transient vision obscurations described as “gray-outs” or “black-outs” of vision for less than 10 seconds, often precipitated by postural change.
Delayed photostress recovery can manifest as binocular TVL in age-related macular degeneration and other bilateral maculopathies.5
Differential diagnosis
Tables 3 and 4 detail the differential diagnosis for monocular and binocular TVL, respectively. Careful history regarding the nature and features of TVL are an important guide to the differential diagnosis of each patient. Monocular vision loss localizes to a prechiasmal or anterior circulation problem; whereas, binocular vision loss implies a chiasmal, retrochiasmal or posterior circulation issue. Be aware that patients experiencing hemifield loss may interpret vision loss as monocular because the involvement of the ipsilateral temporal field is larger than the corresponding nasal field and non-redundant.6 Clarify whether each eye was covered to ascertain laterality. Rarely, bilateral ocular pathology presents as simultaneous TVL.
 Table 3 Click to enlarge |
 Table 4. Click to enlarge |
Seeing lights in the vision, known as positive symptoms, vs. darkening of vision, known as negative symptoms, is another helpful distinction. Purely negative symptoms of vision loss are more likely due to ischemia; whereas, positive symptoms commonly indicate migraine, retinal disease or occipital lobe seizure.4 Positive visual phenomena originate from the retina or the brain. Retinal photopsias are typically unilateral, white, lightening-like flashes that last for less than 1 second. They are often noted with retinal breaks or epiretinal membranes. Neurologic photopsias are generally bilateral, white or colored, positive vision disturbances lasting longer than a few seconds to several minutes.
Symptoms of intracranial noises, pulse-synchronous tinnitus, headache, diplopia, nausea and emesis can point to elevated intracranial pressure.
Giant cell arteritis (GCA) should be of concern in elderly patients with TVL, especially in combination with temporal headache, scalp tenderness or jaw claudication.8
Transient binocular vision loss noted as a small scotoma in homonymous portions of the visual field surrounded by jagged, shimmering edges is called a scintillating scotoma. The scotoma enlarges over 20-30 minutes but no longer than 60 minutes and then gradually disappears. The vision loss may enlarge to a complete homonymous hemianopsia. A hemicranial, throbbing headache, known as a migraine with aura, follows. A migraine aura without headache, formerly known as acephalgic migraine, presents as binocular TVL as described above; no headache follows.9
Vertebrobasilar ischemia can cause complete binocular TVL with both eyes affected equally and at the same time.8 Patients with vertebrobasilar ischemia may also present with other neurologic symptoms such as speech or vestibular deficits. Table 4 details considerations for the underlying etiology.
Retinal or ocular migraine presents with at least two attacks of recurrent, monocular aura similar to classic migraine aura in appearance and progression. The aura is followed by a headache occurring within 60 minutes of the vision disturbance. This group of patients often has a personal or family history of migraine and they are predominantly females younger than 50. This is a diagnosis of exclusion; therefore, workup is warranted.3
Gaze-evoked TVL is indicative of an orbital space-occupying lesion such as cavernous hemangioma, optic nerve sheath meningioma, orbital inflammatory disease, thyroid orbitopathy or foreign body.10 Compression of the orbital vasculature and reduction of blood supply are often monocular in nature.
Carotid artery disease is a common cause of monocular TVL, whether from narrowing due to plaque formation, embolus, plaque ulceration and hemorrhage, carotid trauma or carotid dissection. Recurrent orbital or facial pain that improves when the patient lies down is highly suggestive of carotid occlusive disease. Ultrasound imaging, magnetic resonance angiography (MRA) and CTA can all be used to assess for carotid artery disease. Carotid dissection may be too distal to be visualized on carotid ultrasound; therefore, MRA or CTA of the head and neck is indicated to exclude this diagnosis.4 An ipsilateral Horner syndrome with headache or neck pain indicates a carotid dissection until proven otherwise.6
Other less common causes of insufficient vascular supply to the eye may include stenosis or dissection of the ophthalmic artery, aortic arch atheroma, arteriovenous malformations, intravascular lymphoma, hypercoagulable states, systemic hypotension, vasospasm or vasculitis.8
Management
TVL is a symptom of an underlying disease; therefore, there is no single protocol for treatment. As such, this case report highlights the relevance of collaboration with other members of the healthcare team to most effectively manage the health of the patient. Management is aimed at treating the underlying condition to reduce symptoms and prevent future complications. Depending on the suspected cause and onset of symptoms, this may require emergent referral for stroke protocol initiation, outpatient serology and/or imaging, referral to other specialists, or coordination with the patient’s primary care doctor and the patient to implement appropriate lifestyle changes. The following discussion offers guidance for common causes.
If the ocular examination reveals pathology consistent with an ocular or orbital etiology, the patient should be managed as appropriate. Gaze-evoked TVL warrants neuroimaging with an MRI study preferred.
Patients experiencing central retinal artery occlusion (CRAO) or branch retinal artery occlusion should be carefully followed for the ocular sequelae and undergo emergent stroke protocol at a stroke-certified hospital. Management should also include mitigating other risk factors for stroke such as hypertension, hyperlipidemia and diabetes and implementing lifestyle changes such as tobacco cessation, healthy diet/nutrition, exercise and stress reduction. A study of vascular risk factors and CRAO found that 64% of patients with CRAO had at least one new vascular risk factor that was not known prior to the occlusive event, with hyperlipidemia being the most common.11
In patients presenting with complete monocular TVL (also known as amaurosis fugax), especially with a history of cerebrovascular risk factors, carotid disease should be highly suspected whether retinal emboli are present or not. Approximately 19% of patients with amaurosis fugax were found to have significant carotid stenosis.12 The absence of retinal emboli does not rule out carotid disease. Patients presenting with retinal emboli who are experiencing TVL have a much higher chance of having significant (>69%) carotid artery stenosis than asymptomatic patients with retinal emboli.13 Emergent referral for a stroke workup is warranted for those suspected of TIA or evolving stroke. Patients diagnosed with mild or moderate carotid stenosis are typically managed with anti-platelet medications and lifestyle changes with annual bilateral carotid artery duplex. Carotid artery disease >69% warrants vascular surgery consultation for possible carotid endarterectomy or angioplasty with stenting. When carotid evaluation is normal and a thromboembolic cause is suspected, an echocardiogram and electrocardiogram should be considered to evaluate for a cardioembolic source.1
TVL presenting with head pain, scalp tenderness or jaw claudication is highly suspicious for GCA. Ninety percent of known GCA cases present with ocular signs or symptoms with amaurosis fugax reported in 20-30% of them.14,15 GCA should be a differential in any patient older than 50 with TVL. Important serology testing includes complete blood count with platelet differential, Westergren erythrocyte sedimentation rate, and C-reactive protein. GCA-associated vision loss is often severe, with 43% of cases presenting with transient vision loss resulting in significant permanent vision loss after treatment.16,15 Recognizing early signs and symptoms of GCA prior to sustained vision loss is important for early treatment with steroids and better visual prognosis. With overlap in health and lifestyle risk factors for TVL caused by GCA and carotid disease, all patients presenting with monocular transient vision loss in the setting of cerebrovascular risk factors should be evaluated for both.12
For recurring TVL in which other cerebrovascular testing is normal, a hypercoagulable workup should be considered. Patients at risk for acquired hypercoagulable states include who are immobile, smoke, or have elevated estrogen due to pregnancy or pharmacologic treatments including birth control.1
Retinal migraine or central retinal artery vasospasm should be considered in cases of unilateral TVL in younger patients especially those with history of migraine or Raynaud phenomenon. Retinal migraines respond to traditional migraine management such as NSAIDS, caffeine and triptans, as well as avoidance of lifestyle triggers, if known.17 Calcium channel blockers such as nifedipine or verapamil can be useful for retinal vasospasm management.18
Binocular TVL has a similar differential diagnosis as monocular TVL including thromboembolic causes. Binocular TVL can also be caused by occipital lobe pathology such as ischemia or compressive lesion; therefore, neuroimaging must be considered. In cases where the TVL history and examination are suggestive of TIA or stroke, emergent referral must be made to the emergency department for stroke protocol initiation.
Critical-thinking concepts
How soon should a patient be seen for examination with TVL symptoms? Because the etiology of TVL can range from benign to potentially sight- or life-threatening, emergent ocular examination is warranted. For this reason, it is not only important for the doctor to recognize the significance of TVL symptoms, it is also important for office staff to be well-trained in triaging. In the presence of a normal ocular exam with a high suspicion for vascular cause, emergent referral to the emergency department for stroke protocol initiation is warranted. Effective interprofessional collaboration can be initiated by courtesy phone call to the charge nurse or admitting physician to coordinate timely care and clarify the need for emergency evaluation.
In the case described, what aspects of the patient’s health history were crucial in determining the etiology of TVL? The patient is a 70-year-old Black male with recurrent episodes of monocular, altitudinal TVL associated with angina. Health history was positive for aortic regurgitation, hyperlipidemia and hypertension; family history was positive for coronary artery disease. This history led the clinician to suspect a vascular etiology. Given the vast differential, careful attention to age, race, gender and cardiovascular status can significantly reduce the diagnosis possibilities. Altitudinal TVL is well-known to correlate with a vascular cause. The associated symptom of angina was also key.
What were some of the distinguishing features of the patient’s TVL that helped guide the workup? Alongside the health history, a detailed HPI can help steer the diagnostic process while minimizing unnecessary tests. One of the first and most distinguishing questions to ask in a case of TVL is whether the vision loss is monocular or binocular. Other questions to follow should include the pattern of vision loss and recovery, the duration of symptoms, any known triggers such as light exposure, and any other symptoms associated with onset or resolution. Monocular TVL localizes the pathology to pre-chiasmal structures or the anterior circulation. As in the case presented, the patient’s monocular TVL correlated with a right carotid artery bulb cholesterol plaque. Altitudinal episodes of monocular TVL often have carotid or retinal embolic causes.19
Conclusion
Transient vision loss is a symptom that signals underlying ocular or systemic conditions, some of which are emergent. Because patients with transient vision loss commonly present to eyecare providers, understanding the potential etiologies of vision loss and initiating evaluation and treatment are essential. To preserve life and sight, providers should be able to identify emergent conditions and initiate evaluation protocols including emergency department referral and timely communication with other medical professionals.
References
- Pula JH, Kwan K, Yuen CA, Kattah JC. Update on the evaluation of transient vision loss. Clin Ophthalmol. 2016 Feb 11;10:297-303.
- Tran C, Skorin L. A Workup Protocol for Transient Vision Loss [Internet]. Newtown Square, PA: Review of Optometry; [cited 2020 Sep 26]. Available from: https://www.reviewofoptometry.com/article/a-workup-protocol-for-transient-vision-loss.
- Ahmed R, Foroozan R. Transient monocular visual loss. Neurol Clin. 2010 Aug;28(3):619-29.
- Hamedani AG. In: Decision-making in adult neurology. Elsevier; 2021. Chapter 12, Transient vision loss; p. 24-25.
- Tamhankar MA. In: Liu, Volpe, and Galetta’s neuro-ophthalmology, 3rd ed. Elsevier; 2019. Chapter 10, Transient visual loss or blurring; p. 365-377.
- Thurtell MJ, Rucker JC. Transient visual loss. Int Ophthalmol Clin. 2009 Summer;49(3):147-66.
- Quiros PA, Wang MY. In: Ophthalmology, 5th ed. Elsevier; 2019. Chapter 9.26, Vascular disorders; p. 995-1002.
- Lamirel C, Newman NJ, Biousse V. Vascular neuro-ophthalmology. Handb Clin Neurol. 2009;93:595-611.
- Salmon J. Kanski’s clinical ophthalmology, 9th ed. Elsevier; 2020. Chapter 19, Neuro-ophthalmology; p. 745-825.
- Petzold A, Islam N, Hu HH, Plant GT. Embolic and nonembolic transient monocular visual field loss: a clinicopathologic review. Surv Ophthalmol. 2013 Jan-Feb;58(1):42-62.
- Rudkin AK, Lee AW, Chen CS. Vascular risk factors for central retinal artery occlusion. Eye (Lond). 2010 Apr;24(4):678-81.
- Kvickström P, Lindblom B, Bergström G, Zetterberg M. Amaurosis fugax: risk factors and prevalence of significant carotid stenosis. Clin Ophthalmol. 2016 Oct 31;10:2165-2170.
- Bakri SJ, Luqman A, Pathik B, Chandrasekaran K. Is carotid ultrasound necessary in the evaluation of the asymptomatic Hollenhorst plaque? Ophthalmology. 2013 Dec;120(12):2747-2748.e1.
- Hayreh SS, Podhajsky PA, Zimmerman B. Ocular manifestations of giant cell arteritis. Am J Ophthalmol. 1998 Apr;125(4):509-20.
- Liozon E, Herrmann F, Ly K, Robert PY, Loustaud V, Soria P, Vidal E. Risk factors for visual loss in giant cell (temporal) arteritis: a prospective study of 174 patients. Am J Med. 2001 Aug 15;111(3):211-7.
- Danesh-Meyer H, Savino PJ, Gamble GG. Poor prognosis of visual outcome after visual loss from giant cell arteritis. Ophthalmology. 2005 Jun;112(6):1098-103.
- Istrate BM, Vîlciu C, Răgan C. Retinal migraine. Rom J Ophthalmol. 2020 Apr-Jun;64(2):96-99.
- Pitkänen H, Saarela V. Vasospastic transient monocular visual loss: effect of treatment with different doses of nifedipine. J Neuroophthalmol. 2014 Dec;34(4):386-8.
- Bruno A, Corbett JJ, Biller J, Adams HP Jr, Qualls C. Transient monocular visual loss patterns and associated vascular abnormalities. Stroke. 1990 Jan;21(1):34-9.





